Kurze Zusammenfassung: Die digitale Transformation im Gesundheitswesen integriert fortschrittliche Technologien wie KI, Telemedizin, EHR-Systeme und IoT, um die Patientenversorgung, die betriebliche Effizienz und die klinischen Ergebnisse zu verbessern. Untersuchungen zufolge verfolgen 92% der Gesundheitssysteme die digitale Transformation in erster Linie, um die Patientenerfahrung zu verbessern, während 75% der US-Krankenhäuser jetzt elektronische Systeme verwenden. Mit dieser Umstellung werden kritische Herausforderungen wie Kostensenkung, Datensicherheit und Zugänglichkeit der Versorgung angegangen, während Gesundheitsorganisationen für nachhaltige Innovationen positioniert werden.
Das Gesundheitswesen steht an einem technologischen Scheideweg. Die Branche, die sich einst auf Papiertabellen und persönliche Konsultationen verließ, setzt heute auf künstliche Intelligenz, Fernüberwachung und vorausschauende Analytik.
Aber die Sache ist die: Bei der digitalen Transformation geht es nicht nur um die Einführung neuer Tools. Sie verändert grundlegend die Arbeitsweise von Gesundheitsorganisationen, die Art und Weise, wie Kliniker Entscheidungen treffen und wie Patienten die Versorgung erleben.
Untersuchungen des Forschungsprogramms der Agency for Healthcare Research and Quality, das seit 20 Jahren läuft, zeigen, dass sich dieser Wandel im Laufe der Zeit vollzogen hat. Was mit einfachen elektronischen Aufzeichnungen begann, hat sich zu umfassenden digitalen Ökosystemen entwickelt, die jeden Aspekt der Gesundheitsversorgung betreffen.
Das kanadische Förderprogramm für digitale Gesundheit investierte $42 Mio. CAD in 22 Forschungsteams, was zeigt, dass beträchtliche Mittel in die digitale Gesundheitsinnovation fließen. Die Ergebnisse? Auswirkungen in den Bereichen Kapazitätsentwicklung, Wissensaufbau und evidenzbasierte Entscheidungsfindung.
Dieser umfassende Leitfaden zeigt auf, was die digitale Transformation für Gesundheitsdienstleister bedeutet, welche Technologien den Wandel vorantreiben und welche praktischen Schritte Organisationen unternehmen können, um diese Systeme erfolgreich zu implementieren.
Was die digitale Transformation für das Gesundheitswesen bedeutet
Die digitale Transformation im Gesundheitswesen bezieht sich auf die Integration digitaler Technologien in alle Gesundheitssysteme, um die Art und Weise, wie die Versorgung erbracht, erlebt und verwaltet wird, grundlegend zu verändern.
Im Gegensatz zur einfachen Digitalisierung, bei der Papierunterlagen in elektronische Formate umgewandelt werden, geht es bei der echten Transformation darum, Arbeitsabläufe, Versorgungsmodelle und Patientenbeziehungen mithilfe von Technologie neu zu gestalten.
Nach Angaben der National Academy of Medicine (2026) hinkt das Gesundheitswesen bei der Entwicklung einer robusten digitalen Infrastruktur, die für die vollständige Umsetzung von Innovationen erforderlich ist, im Vergleich zu anderen vernetzten Sektoren weiterhin hinterher. Diese Lücke schränkt die potenziellen Gewinne bei Effizienz, Zugang, Prävention, Diagnose, Behandlung und öffentlichen Gesundheitsergebnissen ein.
Die im International Journal of Environmental Research and Public Health (2023) veröffentlichten Forschungsergebnisse zeigen unter anderem folgende Vorteile auf:
- Gesteigerte Mitarbeiterproduktivität in allen klinischen und administrativen Funktionen
- Verbesserte Effizienz und Effektivität der Arbeit der Gesundheitseinrichtungen
- Senkung der Betriebskosten für Organisationen im Gesundheitswesen
Echtes Gespräch: 75% der US-Krankenhäuser nutzen laut Studien zur Gesundheitsinfrastruktur inzwischen elektronische Gesundheitssysteme. Das ist eine gewaltige Veränderung gegenüber dem Stand der Branche vor nur einem Jahrzehnt.
Der Wandel geht über die internen Abläufe hinaus. Die Gesundheitssysteme überdenken ihre Beziehung zu den Patienten grundlegend. Eine Studie von Deloitte ergab, dass 92% der Befragten eine bessere Patientenerfahrung als wichtigstes Ergebnis der digitalen Transformation nennen.
Der Wandel von der technologiezentrierten zur wertorientierten Versorgung
Die digitale Transformation ermöglicht den Übergang zu einer wertorientierten Gesundheitsversorgung, bei der die Ergebnisse wichtiger sind als die Menge. Technologien stellen die Dateninfrastruktur bereit, die erforderlich ist, um Patientenergebnisse systematisch zu messen, zu verfolgen und zu verbessern.
Laut einer in der Zeitschrift Lancet Regional Health Europe (2021) veröffentlichten Studie spielen digitale Lösungen eine Rolle bei der Förderung wertorientierter Ansätze in der Gesundheitsversorgung und zeigen sowohl Herausforderungen als auch Chancen für Gesundheitsorganisationen auf.
Das bedeutet, dass wir uns nicht mehr nur fragen: “Welche Technologie sollten wir einsetzen?”, sondern: “Wie kann uns die Technologie helfen, bessere Ergebnisse für die Patienten zu erzielen?”
Kerntechnologien für den Wandel im Gesundheitswesen
Mehrere miteinander verknüpfte Technologien bilden die Grundlage für die digitale Transformation im Gesundheitswesen. Das Verständnis der einzelnen Komponenten hilft Organisationen, umfassende digitale Strategien zu entwickeln.
Elektronische Gesundheitsakten und Datenintegration
Elektronische Gesundheitsakten bilden das Rückgrat der digitalen Gesundheitssysteme. Diese Plattformen konsolidieren Patienteninformationen und machen sie autorisierten Anbietern in verschiedenen Versorgungsbereichen zugänglich.
Aber EHR-Systeme entwickeln sich über die einfache Speicherung von Aufzeichnungen hinaus weiter. Moderne Plattformen lassen sich mit Diagnosetools, Behandlungsplanungssystemen und Patientenportalen integrieren, um einen nahtlosen Informationsfluss zu schaffen.
Das 20-jährige AHRQ-Forschungsprogramm zur digitalen Gesundheitsfürsorge betont, dass “digitale Gesundheitsfürsorge” heute für Aktivitäten gilt, die den Informationstransfer während der gesamten Patientenreise und die intelligente Nutzung aller damit verbundenen Daten umfassen.
Das ist ein entscheidender Unterschied. Digitale Transformation bedeutet, Informationssilos aufzubrechen, damit Daten als Entscheidungsgrundlage an jedem Berührungspunkt dienen können.
Künstliche Intelligenz und prädiktive Analytik
KI ist einer der am schnellsten wachsenden Bereiche der digitalen Transformation im Gesundheitswesen. Untersuchungen zeigen, dass 65% der US-Krankenhäuser inzwischen KI-gestützte Vorhersagetools in ihren EHR-Systemen verwenden.
Diese Instrumente helfen den Ärzten:
- Identifizierung von Patienten mit einem Risiko für bestimmte Krankheiten, bevor Symptome auftreten
- Empfehlung von Behandlungspfaden auf der Grundlage ähnlicher Patientenergebnisse
- Mögliche Wechselwirkungen oder Kontraindikationen von Medikamenten anzeigen
- Optimierung der Personal- und Ressourcenzuweisung auf der Grundlage des prognostizierten Patientenaufkommens
Jüngste Forschungsarbeiten zu Technologien der künstlichen Intelligenz und des Internets der Dinge (AIoT) zeigen, wie die Integration nachhaltige Systeme der Gesundheitsversorgung unterstützen kann. Umfassende Bewertungsrahmen sind nun erforderlich, um die Auswirkungen der Technologie auf nachhaltige Ergebnisse der Gesundheitsversorgung zu bewerten.
Der Datenzugriff in Echtzeit beschleunigt und verbessert die Entscheidungsfindung erheblich. Kliniker können auf Erkenntnisse reagieren, deren manuelle Zusammenstellung Tage oder Wochen gedauert hätte.
Telemedizin und Patientenfernüberwachung
Die Ausweitung der telemedizinischen Möglichkeiten hat die Art und Weise und den Ort der Versorgung grundlegend verändert. Patienten können jetzt Facharztkonsultationen, Nachsorgetermine und die Behandlung chronischer Krankheiten in Anspruch nehmen, ohne eine Gesundheitseinrichtung aufsuchen zu müssen.
Die Fernüberwachung von Patienten geht noch einen Schritt weiter, indem sie kontinuierlich Gesundheitsdaten über tragbare Geräte und Heimüberwachungsanlagen erfasst. Dies schafft Möglichkeiten für frühzeitiges Eingreifen und proaktives Pflegemanagement.
Digitale Innovationen verbessern den gleichberechtigten Zugang zu den Gesundheitssystemen, verbessern die Integration der Versorgung und unterstützen lernende Gesundheitssysteme, wie Untersuchungen zu Finanzierungsprogrammen für digitale Gesundheit zeigen.
Internet der Dinge und vernetzte medizinische Geräte
Die IoT-Technologie verbindet medizinische Geräte, Monitore und Sensoren, um umfassende Ökosysteme zur Gesundheitsüberwachung zu schaffen. Diese Geräte erfassen in Echtzeit physiologische Daten, Umgebungsbedingungen und Verhaltensmuster der Patienten.
In Krankenhäusern ermöglicht das IoT die Nachverfolgung von Vermögenswerten, die Überwachung der Umgebung und ein automatisiertes Lieferkettenmanagement. Für Patienten zu Hause unterstützen vernetzte Geräte ein unabhängiges Leben und versorgen klinische Teams mit kontinuierlichen Gesundheitsdaten.
Die Integration von KI und IoT schafft besonders leistungsfähige Möglichkeiten für eine nachhaltige Gesundheitsversorgung und Patientenergebnisse.
Datenanalyse und Business Intelligence
Moderne Analyseplattformen verwandeln riesige Datenmengen im Gesundheitswesen in verwertbare Erkenntnisse. Unternehmen können Versorgungsmuster erkennen, die Wirksamkeit von Maßnahmen messen und die betriebliche Leistung optimieren.
Das Population Health Management stützt sich in hohem Maße auf Analysen, um Risikogruppen zu identifizieren, Krankheitstrends vorherzusagen und Präventionsressourcen effektiv zuzuweisen.
Laut einer Analyse von Stellenausschreibungsdaten gab es von 2017 bis 2022 einen Zuwachs von 35,5% bei den Berufen im Gesundheitsmanagement, was die erhöhte Nachfrage nach Fachkräften widerspiegelt, die eine Brücke zwischen Technologie und Gesundheitsbetrieb schlagen können.
| Technologie | Primäre Funktion | Wichtigste Vorteile | Herausforderung Adoption |
|---|---|---|---|
| Elektronische Gesundheitsakten | Zentralisierte Patientendaten | Zugänglichkeit von Informationen, Koordinierung der Pflege | Interoperabilität zwischen Systemen |
| KI und prädiktive Analytik | Entscheidungshilfe, Risikovorhersage | Frühzeitiges Eingreifen, personalisierte Behandlung | Datenqualität und Algorithmusverzerrung |
| Telemedizin | Fernbetreuung | Zugang, Bequemlichkeit, Kostensenkung | Digitale Kompetenz und Konnektivität |
| IoT Medizinische Geräte | Kontinuierliche Überwachung | Daten in Echtzeit, proaktive Pflege | Sicherheit und Datenschutz |
| Datenanalyse | Generierung von Einblicken | Leistungsoptimierung, Trenderkennung | Qualifikationsdefizit und Infrastruktur |
Strategische Vorteile der digitalen Transformation
Die Vorteile der digitalen Transformation erstrecken sich auf klinische, betriebliche und finanzielle Aspekte. Organisationen, die digitale Strategien erfolgreich umsetzen, sehen Verbesserungen in mehreren Bereichen gleichzeitig.
Verbessertes Patientenerlebnis und Engagement
Die Patientenerfahrung steht ganz oben auf der Prioritätenliste von Gesundheitssystemen, die eine digitale Transformation anstreben. Technologien ermöglichen einen bequemeren Zugang, eine personalisierte Kommunikation und eine stärkere Einbeziehung der Patienten in Versorgungsentscheidungen.
Digitale Portale ermöglichen den Patienten rund um die Uhr den Zugriff auf Gesundheitsdaten, Testergebnisse und den sicheren Nachrichtenaustausch mit dem Pflegeteam. Mobile Apps unterstützen die Einhaltung von Medikamenten, die Planung von Terminen und die Verfolgung von Symptomen.
Diese Verlagerung hin zu patientenzentrierten digitalen Werkzeugen verwandelt die traditionelle Beziehung zwischen Anbieter und Patient grundlegend in eine stärker kooperative Partnerschaft.
Verbesserte klinische Ergebnisse und Qualität der Pflege
Die digitale Transformation ermöglicht genauere Diagnosen, personalisierte Behandlungen und evidenzbasierte Interventionen. Systeme zur Unterstützung klinischer Entscheidungen verringern medizinische Fehler, indem sie potenzielle Probleme erkennen, bevor sie Patienten schaden.
Untersuchungen zu digitalen Krankenhäusern zeigen, dass Kliniker über positive Erfahrungen mit Indikatoren wie Gesamtzufriedenheit und Datenzugänglichkeit berichten, obwohl qualitative Daten Spannungen aufzeigen, die die Organisationen angehen müssen.
Kontinuierliche Überwachung und prädiktive Analysen ermöglichen eine frühere Erkennung einer Verschlechterung des Zustands und damit rechtzeitige Eingriffe, die die Ergebnisse verbessern und Komplikationen verringern.
Betriebliche Effizienz und Kostenreduzierung
Digitale Tools rationalisieren die Verwaltungsprozesse, reduzieren redundante Tests und optimieren die Ressourcenzuweisung. Automatisierte Arbeitsabläufe machen manuelle Aufgaben überflüssig, die dem Personal Zeit rauben, ohne klinischen Nutzen zu bringen.
Studien zeigen immer wieder, dass die Verbesserung der betrieblichen Effizienz zu den wichtigsten Vorteilen der digitalen Transformation zählt. Unternehmen berichten von geringeren Betriebskosten und einer verbesserten Leistungserbringung.
Die Optimierung der Lieferkette, die vorausschauende Wartung medizinischer Geräte und die intelligente Terminplanung tragen zu Kosteneinsparungen bei, die in die Patientenversorgung fließen können.
Datengestützte Entscheidungsfindung
Der Zugang zu umfassenden Echtzeitdaten verändert die Art und Weise, wie Führungskräfte im Gesundheitswesen strategische Entscheidungen treffen. Analysen decken Muster auf, die in fragmentierten, manuellen Systemen unsichtbar bleiben würden.
Unternehmen können die Wirksamkeit spezifischer Maßnahmen messen, die Leistung verschiedener Abteilungen vergleichen und Verbesserungsmöglichkeiten auf der Grundlage objektiver Nachweise und nicht auf der Grundlage von Annahmen ermitteln.
Diese Fähigkeit ist besonders wertvoll für Initiativen zur Qualitätsverbesserung und zur Einhaltung von Vorschriften.
Produktivität und Zufriedenheit der Mitarbeiter
Die digitale Transformation erfordert zwar das Erlernen neuer Systeme, doch Untersuchungen zeigen, dass sie letztlich die Produktivität der Mitarbeiter erhöht. Durch die Automatisierung von Routineaufgaben kann sich das Klinikpersonal auf Tätigkeiten konzentrieren, die menschliches Urteilsvermögen und Einfühlungsvermögen erfordern.
Digitale Tools können den Dokumentationsaufwand verringern, die Kommunikation optimieren und Entscheidungshilfen bieten, die die Arbeit der Ärzte effektiver und zufriedenstellender machen.
Allerdings ist die Umsetzung von enormer Bedeutung. Schlecht konzipierte Systeme oder unzureichende Schulungen können eher zu Frustration als zu Produktivitätssteigerungen führen.
Kritische Herausforderungen bei der Implementierung
Die digitale Transformation verspricht erhebliche Vorteile, doch die Umsetzung ist mit erheblichen Herausforderungen verbunden. Die Kenntnis dieser Hindernisse hilft Unternehmen bei der Planung realistischer Strategien.
Bedenken hinsichtlich der Datensicherheit und des Datenschutzes
Daten aus dem Gesundheitswesen sind ein attraktives Ziel für Cyberkriminelle. Die digitale Transformation vergrößert die Angriffsfläche, da mehr Systeme miteinander verbunden sind und mehr Daten über Netzwerke übertragen werden.
Die Forschung zu digitaler Sicherheit und Governance unterstreicht, dass solide Governance-Rahmen für eine sichere, gerechte und nachhaltige Umsetzung der digitalen Gesundheit bei gleichzeitiger Minderung der Cybersicherheitsrisiken unerlässlich sind.
Unternehmen müssen ein Gleichgewicht zwischen Zugänglichkeit und Sicherheit herstellen, indem sie Daten für autorisierte Benutzer verfügbar machen und sie gleichzeitig vor unbefugtem Zugriff, Sicherheitsverletzungen und Ransomware-Angriffen schützen.
Regulatorische Anforderungen wie HIPAA erhöhen die Komplexität und erfordern eine sorgfältige Prüfung, wie Daten während ihres gesamten Lebenszyklus erfasst, gespeichert, übertragen und entsorgt werden.
Interoperabilität und Systemintegration
Organisationen des Gesundheitswesens arbeiten in der Regel mit mehreren Systemen verschiedener Anbieter. Die effektive Kommunikation dieser Systeme ist nach wie vor eine der größten technischen Herausforderungen.
Mangelnde Standardisierung bedeutet, dass Daten, die für ein System formatiert wurden, möglicherweise nicht sauber in ein anderes übertragen werden können. Kritische Informationen können bei der Übersetzung verloren gehen oder erfordern manuelle Eingriffe, um sie abzugleichen.
Die National Academy of Medicine weist darauf hin, dass die Entwicklung einer robusten digitalen Gesundheitsinfrastruktur die Behebung dieser Interoperabilitätslücken erfordert, die Effizienz und Innovation einschränken.
Technologieakzeptanz und Änderungsmanagement
Untersuchungen zur Technologieakzeptanz bei der Umgestaltung des Gesundheitswesens haben gezeigt, dass die erfolgreiche Umsetzung stark davon abhängt, wie gut Organisationen die menschliche Seite des Wandels bewältigen.
Das klinische Personal sträubt sich unter Umständen gegen neue Systeme, die die etablierten Arbeitsabläufe stören oder die tägliche Routine komplizierter erscheinen lassen. Ohne angemessene Schulung und Unterstützung kann selbst eine gut konzipierte Technologie nicht den erwarteten Nutzen bringen.
Strategien zur Bewältigung des Wandels müssen auf Bedenken eingehen, angemessene Schulungen anbieten und den Nutzern, die letztlich über Erfolg oder Misserfolg digitaler Werkzeuge entscheiden, den Wert dieser Instrumente aufzeigen.
Qualifikationsdefizit und Entwicklung der Arbeitskräfte
Die digitale Transformation erfordert Fähigkeiten, an denen es vielen Organisationen im Gesundheitswesen intern mangelt. Datenwissenschaftler, Cybersicherheitsspezialisten, digitale Strategen und IT-Architekten sind weiterhin sehr gefragt.
Die Zunahme der Berufe im Gesundheitsmanagement spiegelt die zunehmende Erkenntnis wider, dass eine erfolgreiche digitale Transformation Fachleute erfordert, die sowohl das Gesundheitswesen als auch die Technologie verstehen.
Die Unternehmen müssen entscheiden, ob sie interne Fähigkeiten durch Schulungen und Einstellungen aufbauen, mit externen Spezialisten zusammenarbeiten oder einen gemischten Ansatz wählen.
Finanzielle Investitionen und ROI-Ungewissheit
Die digitale Transformation erfordert erhebliche Vorabinvestitionen in Technologie, Schulungen und organisatorische Veränderungen. Die Vorteile kommen oft erst nach einiger Zeit zum Tragen, was zu einem Spannungsverhältnis zwischen kurzfristigen Kosten und langfristigem Nutzen führt.
Die Messung der Investitionsrendite kann eine Herausforderung sein, wenn die Vorteile nicht nur unmittelbare Kosteneinsparungen, sondern auch immaterielle Faktoren wie eine verbesserte Patientenzufriedenheit oder eine Verringerung künftiger Komplikationen umfassen.
Budgetbeschränkungen zwingen Unternehmen dazu, Initiativen sorgfältig zu priorisieren und zwischen schnellen Erfolgen und strategischen Fähigkeiten abzuwägen, deren vollständige Umsetzung Jahre dauern kann.
Einhaltung von Vorschriften und Governance
Das Gesundheitswesen befindet sich in einem stark regulierten Umfeld. Initiativen zur digitalen Transformation müssen Datenschutzgesetze, Sicherheitsstandards, Erstattungsanforderungen und berufsrechtliche Vorschriften einhalten.
Untersuchungen zeigen, dass die digitale Transformation zwar positiv gesehen wird, aber noch erhebliche Lücken bei der Einführung, der Schulung und den Governance-Rahmenbedingungen bestehen. Die Behebung dieser Lücken ist für eine sichere, gerechte und nachhaltige Umsetzung der digitalen Gesundheit unerlässlich.
Der Governance-Rahmen muss sich parallel zur Technologie weiterentwickeln, um eine angemessene Aufsicht zu gewährleisten, ohne die Innovation zu behindern.
| Herausforderung | Auswirkungen | Strategie zur Risikominderung |
|---|---|---|
| Datensicherheit | Verletzungsrisiko, Verstöße gegen die Vorschriften | Robuste Cybersicherheit, Mitarbeiterschulung, Governance-Rahmen |
| Interoperabilität | Informationssilos, Ineffizienz | Standardprotokolle, API-Integration, Anbieterkoordination |
| Veränderungswiderstand | Geringe Akzeptanz, Unterbrechung der Arbeitsabläufe | Änderungsmanagement, Schulung, Einbeziehung der Nutzer in die Gestaltung |
| Qualifikationsdefizit | Verzögerungen bei der Umsetzung, suboptimale Nutzung | Gezielte Neueinstellungen, Personalentwicklung, Partnerschaften |
| Finanzielle Zwänge | Begrenzter Anwendungsbereich, verzögerte Umsetzung | Schrittweiser Ansatz, ROI-Demonstration, Zuschussfinanzierung |
| Einhaltung von Vorschriften | Rechtliche Risiken, Projektverzögerungen | Integration von Compliance, rechtliche Überprüfung, Governance-Struktur |
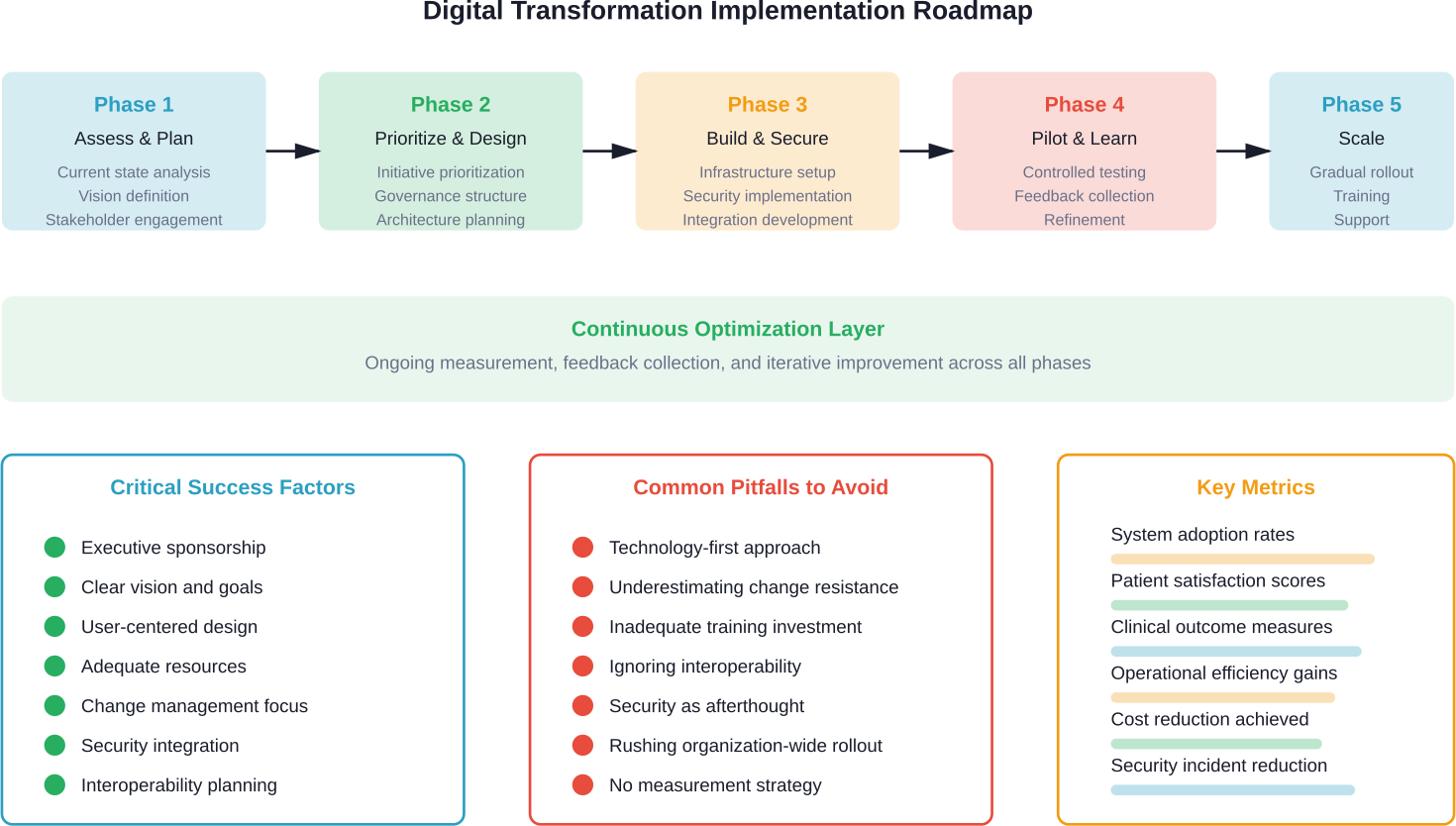
Strategischer Fahrplan für die Umsetzung
Eine erfolgreiche digitale Transformation erfordert eine durchdachte Planung und schrittweise Umsetzung. Unternehmen, die die Umsetzung überstürzen, müssen oft mit kostspieligen Rückschlägen und dem Widerstand der Nutzer rechnen.
Bewertung des aktuellen Zustands und Definition der Vision
Beginnen Sie mit einer ehrlichen Bewertung der vorhandenen digitalen Fähigkeiten, der Infrastruktur und der organisatorischen Bereitschaft. Ermitteln Sie die Lücken zwischen dem aktuellen Zustand und den gewünschten Ergebnissen.
Definieren Sie eine klare Vision, was mit der digitalen Transformation erreicht werden soll. Diese Vision sollte mit strategischen Zielen wie der Verbesserung der Patientenergebnisse, der Erweiterung des Zugangs oder der Kostensenkung verbunden sein.
Beziehen Sie die Interessengruppen in der gesamten Organisation ein - Ärzte, Administratoren, IT-Mitarbeiter und Patienten -, um die Bedürfnisse, Anliegen und Prioritäten aus verschiedenen Perspektiven zu verstehen.
Priorisierung von Initiativen auf der Grundlage von Wert und Durchführbarkeit
Nicht alle digitalen Initiativen sind von gleichem Wert oder stehen vor den gleichen Herausforderungen bei der Umsetzung. Bilden Sie potenzielle Projekte entlang zweier Dimensionen ab: erwartete Auswirkungen und Umsetzungsschwierigkeiten.
Schnelle Erfolge - Projekte mit hohem Wert und geringem Schwierigkeitsgrad - schaffen eine Dynamik und zeigen die Vorteile der digitalen Transformation. Diese frühen Erfolge schaffen Unterstützung für komplexere Initiativen.
Strategische Grundlagen - Fähigkeiten, die künftige Innovationen ermöglichen, auch wenn der unmittelbare Nutzen bescheiden ist - sind trotz längerer Fristen investitionswürdig.
Entwicklung von Governance- und Change-Management-Strukturen
Legen Sie eine klare Governance für digitale Initiativen fest. Wer trifft Entscheidungen über Technologieinvestitionen? Wie werden Prioritäten gesetzt? Welche Prozesse gewährleisten die Einhaltung der Vorschriften und das Risikomanagement?
Das Änderungsmanagement sollte von Anfang an integriert werden und nicht erst nachträglich hinzugefügt werden. Planen Sie Kommunikation, Schulung, Unterstützung und die Sammlung von Feedback während der gesamten Umsetzung.
Die Forschung zu digitaler Sicherheit und Governance unterstreicht, dass robuste Governance-Rahmenwerke für eine sichere, gerechte und nachhaltige Umsetzung der digitalen Gesundheit unerlässlich sind.
Investitionen in Infrastruktur und Sicherheit
Die digitale Transformation erfordert eine robuste Infrastruktur - Netze, Server, Sicherheitssysteme und Integrationsplattformen. Zu geringe Investitionen in diese Grundlagen unterminieren die darauf aufbauenden Anwendungen.
Sicherheit kann nicht nachträglich aufgeschraubt werden. Bauen Sie die Sicherheit von Anfang an in Architektur, Prozesse und Kultur ein.
Die Cloud-Infrastruktur bietet Skalierbarkeit und geringere Investitionen, bringt aber auch neue Überlegungen zur Datenhoheit und Anbieterabhängigkeit mit sich.
Pilot, Lernen und Skalieren
Testen Sie neue Technologien und Arbeitsabläufe in einem kontrollierten Umfeld, bevor Sie sie unternehmensweit einführen. Dies ermöglicht Tests, Verfeinerungen und Kurskorrekturen bei begrenztem Risiko.
Sammeln Sie systematisch Feedback von den Pilotteilnehmern. Was funktioniert gut? Was erzeugt Reibungen? Wie könnte die Umsetzung verbessert werden?
Erfolgreiche Pilotprojekte sollten schrittweise ausgeweitet werden, wobei die gewonnenen Erkenntnisse in jeder Erweiterungsphase zu berücksichtigen sind. Eine überstürzte unternehmensweite Einführung, bevor die Probleme gelöst sind, geht oft nach hinten los.
Messen, Optimieren und Iterieren
Definieren Sie Messgrößen, die sowohl den Fortschritt bei der Umsetzung als auch das Erreichen der Ergebnisse verfolgen. Werden die Systeme wie beabsichtigt eingeführt? Bringen sie den erwarteten Nutzen?
Die digitale Transformation ist kein einmaliges Projekt, sondern ein fortlaufender Prozess. Die Technologien entwickeln sich weiter, die Bedürfnisse ändern sich, und es ergeben sich ständig neue Optimierungsmöglichkeiten.
Schaffen Sie Feedbackschleifen, die eine kontinuierliche Verbesserung ermöglichen, anstatt die Implementierung als abgeschlossen zu betrachten, sobald die Systeme in Betrieb sind.
Starten Sie die digitale Transformation im Gesundheitswesen mit A-listware
Organisationen des Gesundheitswesens arbeiten oft mit Systemen, die vor Jahren entwickelt wurden und nie für die Unterstützung moderner digitaler Dienste konzipiert waren. Die Daten befinden sich möglicherweise auf separaten Plattformen, interne Tools lassen sich nicht gut integrieren, und die Aktualisierung von Altsoftware kann den täglichen Betrieb verlangsamen. A-listware arbeitet mit Gesundheitsdienstleistern und Technologieunternehmen im Gesundheitswesen zusammen, die praktische Unterstützung bei der Modernisierung dieser Systeme benötigen. Die Techniker von A-listware helfen bei der Überprüfung der bestehenden Infrastruktur, bei der Entwicklung maßgeschneiderter Software für das Gesundheitswesen, bei der Migration von Plattformen in die Cloud und bei der Verknüpfung von Systemen, die zuvor getrennt arbeiteten.
Anstatt einen kompletten Neuaufbau zu erzwingen, konzentrieren sich die Projekte in der Regel auf die schrittweise Verbesserung der aktuellen Umgebung. Dies kann die Modernisierung älterer medizinischer Plattformen, die Entwicklung neuer Gesundheitsanwendungen, die Verbesserung von Daten-Workflows oder die Erweiterung der Entwicklungskapazitäten interner Teams umfassen. Wenn Ihre Organisation im Gesundheitswesen eine Initiative zur digitalen Transformation plant und erfahrene Ingenieure für die Umsetzung benötigt, wenden Sie sich an A-listware und besprechen das Projekt mit ihrem Team.
Praktische Anwendungen und Anwendungsfälle
Der digitale Wandel zeigt sich in den verschiedenen Bereichen des Gesundheitswesens unterschiedlich. Das Verständnis praktischer Anwendungen hilft Organisationen, relevante Chancen zu erkennen.
Digitale Transformation von Krankenhäusern und Gesundheitssystemen
Große Gesundheitssysteme führen umfassende digitale Strategien ein, die alle Abteilungen betreffen. EHR-Systeme werden mit Laborinformationssystemen, Radiologieplattformen, Apothekenmanagement und Abrechnungssystemen integriert.
Digitale Krankenhäuser nutzen Technologien zur Optimierung des Patientenflusses, zum vorausschauenden Kapazitätsmanagement und zur automatischen klinischen Dokumentation. Echtzeit-Dashboards geben Administratoren einen Überblick über die Abläufe in mehreren Einrichtungen.
Untersuchungen über die Auswirkungen digitaler Krankenhäuser zeigen, dass Kliniker über positive Erfahrungen mit Indikatoren wie Gesamtzufriedenheit und Datenzugänglichkeit berichten, obwohl qualitative Daten Spannungen aufzeigen, die für einen nachhaltigen Erfolg angegangen werden müssen.
Primärversorgung und ambulante Einrichtungen
Hausarztpraxen nutzen digitale Tools, um Patientengruppen zu verwalten, die Versorgung durch verschiedene Fachärzte zu koordinieren und Programme zur Behandlung chronischer Krankheiten zu unterstützen.
Patientenportale ermöglichen sichere Nachrichtenübermittlung, Terminvergabe und Medikamenteneinnahme ohne Telefonanrufe. Die Telemedizin erweitert den Zugang für Patienten in ländlichen Gebieten oder für Patienten mit Mobilitätseinschränkungen.
Datenanalysen helfen dabei, Patienten zu identifizieren, bei denen Vorsorgeuntersuchungen überfällig sind oder bei denen ein Risiko für Komplikationen besteht, so dass eine proaktive statt einer reaktiven Versorgung möglich ist.
Spezialisierte Pflege und Präzisionsmedizin
Spezialisierte Versorgungszentren nutzen die digitale Transformation, um personalisierte Behandlungen auf der Grundlage von individuellen Patientenmerkmalen, genetischen Profilen und Daten zum Ansprechen auf die Behandlung anzubieten.
KI-gestützte Diagnosetools helfen Radiologen bei der Erkennung feiner Anomalien, Pathologen bei der Klassifizierung von Gewebeproben und Onkologen bei der Auswahl optimaler Behandlungsprotokolle.
Die Forschung zeigt, dass digitale Innovationen genauere Diagnosen und personalisierte Behandlungen ermöglichen und so die Ergebnisse bei komplexen Erkrankungen verbessern.
Anwendungen in der Intensivpflege und auf der Intensivstation
Intensivstationen profitieren besonders von der digitalen Transformation durch Patientendatenmanagementsysteme, die Echtzeitüberwachung, klinische Entscheidungshilfen und standardisierte Dokumentation integrieren.
In Studien zur digitalen Transformation in der Intensivpflege wird untersucht, ob die Einführung dieser integrierten Systeme die Sicherheit und Effizienz der Patienten erhöht.
Die kontinuierliche Überwachung in Kombination mit prädiktiver Analytik kann Kliniker auf eine Verschlechterung des Zustands aufmerksam machen, bevor es zu einem kritischen Notfall kommt.
Öffentliche Gesundheit und Bevölkerungsmanagement
Gesundheitsbehörden nutzen digitale Tools, um Krankheitsausbrüche zu verfolgen, Impfkampagnen zu koordinieren und Gesundheitsmaßnahmen auf Bevölkerungsebene zu verwalten.
Forschungsprogramme zur digitalen Gesundheit, wie die 20-jährige Initiative der AHRQ, fördern Innovationen und Entdeckungen, die neben der Verbesserung der klinischen Versorgung auch die Prioritäten der öffentlichen Gesundheit unterstützen.
Die Analyse der Gesundheit der Bevölkerung ermittelt soziale Gesundheitsfaktoren, gesundheitliche Ungleichheiten und Möglichkeiten für gezielte Maßnahmen zur Verbesserung der Gesundheitsergebnisse in der Gemeinschaft.
Zukünftige Trends und aufkommende Chancen
Die digitale Transformation entwickelt sich weiter, da neue Technologien reifen und sich die Anforderungen im Gesundheitswesen ändern. Mehrere Trends werden die nächste Phase der Digitalisierung des Gesundheitswesens bestimmen.
Fortgeschrittene AI- und Machine Learning-Anwendungen
Die Möglichkeiten der KI werden sich über die derzeitigen Anwendungen hinaus auf Bereiche wie die Entdeckung von Arzneimitteln, die Vorhersage von Behandlungserfolgen und die automatische Diagnoseunterstützung in allen medizinischen Fachbereichen ausweiten.
Modelle des maschinellen Lernens, die auf riesigen Datensätzen trainiert werden, werden Muster erkennen, die Menschen nicht erkennen können, und so möglicherweise neue Ansätze für die Prävention und Behandlung von Krankheiten aufzeigen.
Aber KI wirft auch ethische Fragen zu algorithmischer Voreingenommenheit, klinischer Verantwortung und Patientenautonomie auf, mit denen die Gesundheitssysteme sorgfältig umgehen müssen.
Genomische Medizin und digitale Gesundheitsintegration
Die Integration genomischer Daten mit klinischen Informationen schafft Möglichkeiten für eine wirklich personalisierte Medizin auf der Grundlage individueller genetischer Profile.
Digitale Plattformen, die genetische Informationen, Umweltfaktoren, Daten über den Lebensstil und die Krankengeschichte kombinieren, werden präzise Präventions- und Behandlungsstrategien ermöglichen.
Die Herausforderung besteht darin, die Komplexität der genomischen Daten zu bewältigen und die Erkenntnisse in umsetzbare klinische Empfehlungen zu übersetzen.
Blockchain für das Datenmanagement im Gesundheitswesen
Die Blockchain-Technologie bietet potenzielle Lösungen für den sicheren Austausch von Gesundheitsinformationen, das Eigentum an Patientendaten und die Transparenz der Lieferkette.
Dezentralisierte Architekturen könnten den Patienten mehr Kontrolle über ihre Gesundheitsdaten geben und gleichzeitig die Sicherheit und Interoperabilität zwischen den Systemen gewährleisten.
Allerdings stehen Blockchain-Implementierungen vor technischen und regulatorischen Herausforderungen sowie Problemen bei der Akzeptanz, die eine breite Einführung bisher verhindert haben.
Virtuelle und erweiterte Realität in der medizinischen Ausbildung
VR- und AR-Technologien verändern die medizinische Ausbildung und das chirurgische Training, indem sie immersive Simulationsumgebungen für die Entwicklung von Fähigkeiten ohne Patientenrisiko schaffen.
Chirurgen können komplexe Eingriffe üben, Medizinstudenten können die Anatomie in drei Dimensionen erforschen, und Kliniker können in realistischen Szenarien Notfallmaßnahmen üben.
Diese Technologien unterstützen auch die Patientenaufklärung, indem sie den Menschen helfen, ihre Krankheiten und Behandlungsmöglichkeiten durch visuelle Erfahrungen zu verstehen.
Nationale digitale Gesundheitsinfrastruktur
Die National Academy of Medicine hat ein Diskussionspapier (9. März 2026) zum Aufbau einer nationalen Architektur für digitale Gesundheit und Daten veröffentlicht, die die Grundlage für eine umfassende digitale Transformation bildet.
In dieser Vision wird anerkannt, dass das Gesundheitswesen bei der Entwicklung einer robusten digitalen Infrastruktur, die für die vollständige Umsetzung von Innovationen in den Bereichen Effizienz, Zugang, Prävention, Diagnose, Behandlung und öffentliche Gesundheit erforderlich ist, weiterhin im Rückstand ist.
Eine koordinierte nationale Infrastruktur könnte die Innovation beschleunigen und gleichzeitig die Interoperabilität, Sicherheit und den gleichberechtigten Zugang im gesamten Gesundheitswesen gewährleisten.
Aufbau nachhaltiger digitaler Gesundheitssysteme
Langfristiger Erfolg erfordert ein Denken, das über einzelne Technologieimplementierungen hinausgeht, um nachhaltige digitale Gesundheitsökosysteme zu schaffen.
Ökologische und wirtschaftliche Nachhaltigkeit
Die Forschung zur nachhaltigen Gesundheitsversorgung durch KIoT-Technologie unterstreicht die Notwendigkeit umfassender Bewertungsrahmen, die neben den klinischen und betrieblichen Vorteilen auch die Umweltauswirkungen bewerten.
Digitale Systeme verbrauchen Energie, erzeugen Elektroschrott und erfordern laufende Investitionen in Ressourcen. Die Nachhaltigkeitsplanung sollte neben dem klinischen Wert auch diese Faktoren berücksichtigen.
Wirtschaftliche Nachhaltigkeit erfordert den Nachweis eines dauerhaften Nutzens, der kontinuierliche Investitionen in die Wartung, Aktualisierung und Erweiterung der Technologie rechtfertigt.
Überlegungen zu Gerechtigkeit und Zugang
Der digitale Wandel birgt die Gefahr, dass gesundheitliche Ungleichheiten zunehmen, wenn Technologien nur für gut ausgestattete Organisationen oder digital gebildete Bevölkerungsgruppen zugänglich sind.
Eine gerechte Umsetzung setzt voraus, dass man sich mit der digitalen Kompetenz, der Verbindungsinfrastruktur, den Sprachbarrieren und den Anforderungen an die Zugänglichkeit für Menschen mit Behinderungen befasst.
Die Forschung unterstreicht, dass digitale Innovationen das Potenzial haben, den gleichberechtigten Zugang zu den Gesundheitssystemen zu verbessern, wenn sie mit Bedacht eingesetzt werden.
Ethischer Rahmen für die digitale Gesundheit
Mit der zunehmenden Digitalisierung des Gesundheitswesens müssen die ethischen Rahmenbedingungen weiterentwickelt werden, um neue Fragen zu Dateneigentum, algorithmischer Transparenz, informierter Zustimmung und klinischem Urteilsvermögen zu klären.
Die Forschung zu den Auswirkungen der digitalen Transformation im Gesundheitswesen zeigt sowohl positive klinische Ansichten als auch erhebliche Lücken in der Governance, die für eine sichere und gerechte Umsetzung der digitalen Gesundheit behoben werden müssen.
Unternehmen brauchen klare ethische Richtlinien für den Einsatz von KI, die gemeinsame Nutzung von Daten, den Schutz der Privatsphäre von Patienten und den Ausgleich zwischen Automatisierung und menschlichem Urteilsvermögen bei klinischen Entscheidungen.
Häufig gestellte Fragen
- Was ist die digitale Transformation im Gesundheitswesen?
Die digitale Transformation im Gesundheitswesen ist die umfassende Integration digitaler Technologien in die Gesundheitssysteme, um die Art und Weise, wie die Versorgung erbracht, verwaltet und erlebt wird, grundlegend zu verändern. Dabei geht es nicht nur um die Digitalisierung von Papierakten, sondern auch um die Neugestaltung von Arbeitsabläufen, klinischen Prozessen und Patientenbeziehungen durch Technologien wie KI, Telemedizin, IoT und Datenanalyse. Untersuchungen zufolge verfolgen 92% der Gesundheitssysteme die digitale Transformation in erster Linie, um die Patientenerfahrung zu verbessern und gleichzeitig die betriebliche Effizienz und die klinischen Ergebnisse zu steigern.
- Was sind die wichtigsten Vorteile der digitalen Transformation für Organisationen im Gesundheitswesen?
Zu den wichtigsten Vorteilen gehören ein verbessertes Patientenerlebnis und -engagement, verbesserte klinische Ergebnisse durch datengestützte Entscheidungshilfen, betriebliche Effizienzsteigerungen, geringere Kosten und eine höhere Mitarbeiterproduktivität. Untersuchungen zeigen, dass 75% der US-Krankenhäuser inzwischen elektronische Gesundheitssysteme verwenden, während 65% KI-gestützte Vorhersagetools in ihren EHR-Plattformen einsetzen. Die Organisationen berichten über eine bessere Koordination der Pflege, eine frühere Erkennung von Krankheiten, personalisierte Behandlungsmöglichkeiten und rationalisierte Verwaltungsprozesse als wichtigste Ergebnisse.
- Welche Technologien sind für die digitale Transformation im Gesundheitswesen unerlässlich?
Zu den Kerntechnologien gehören elektronische Gesundheitsakten für zentralisierte Patientendaten, künstliche Intelligenz und prädiktive Analysen zur Entscheidungsunterstützung, telemedizinische Plattformen für die Fernversorgung, Geräte des Internets der Dinge für die kontinuierliche Überwachung und Datenanalysetools zur Gewinnung von Erkenntnissen. Diese Technologien arbeiten als integriertes Ökosystem zusammen und nicht als Einzellösungen. Sicherheitsinfrastrukturen und Interoperabilitätsplattformen sind ebenso wichtig, um einen sicheren und effektiven Datenaustausch zwischen den Systemen zu gewährleisten.
- Was sind die größten Herausforderungen bei der Umsetzung der digitalen Transformation?
Zu den wichtigsten Herausforderungen gehören Bedenken hinsichtlich der Datensicherheit und des Datenschutzes, Probleme mit der Interoperabilität verschiedener Systeme, die Akzeptanz der Technologie und der Widerstand der Mitarbeiter gegen Veränderungen, Qualifikationsdefizite, die spezielles Fachwissen erfordern, erhebliche finanzielle Investitionen mit ungewissem ROI-Zeitrahmen und komplexe gesetzliche Anforderungen. Untersuchungen zeigen, dass die digitale Transformation zwar positiv gesehen wird, dass es aber noch erhebliche Lücken bei der Einführung, Schulung und den für eine nachhaltige Umsetzung erforderlichen Governance-Rahmenbedingungen gibt.
- Wie lange dauert die digitale Transformation im Gesundheitswesen?
Die digitale Transformation ist ein fortlaufender Prozess und nicht ein einzelnes Projekt mit einem festen Endpunkt. Die ersten Implementierungen können je nach Umfang und Bereitschaft des Unternehmens 12 bis 36 Monate dauern, aber die kontinuierliche Optimierung und Weiterentwicklung geht unbegrenzt weiter, da sich die Technologien weiterentwickeln und die Anforderungen ändern. Erfolgreiche Organisationen verfolgen einen stufenweisen Ansatz und beginnen mit Pilotprogrammen, die den Nutzen nachweisen, bevor sie das gesamte System skalieren. Im Rahmen des kanadischen Förderprogramms für digitale Gesundheit wurden 22 Forschungsteams über mehrere Jahre hinweg unterstützt, was den langfristigen Charakter der Transformationsbemühungen widerspiegelt.
- Wie können Organisationen im Gesundheitswesen den Erfolg der digitalen Transformation messen?
Unternehmen sollten mehrere Messgrößen aus dem klinischen, betrieblichen und finanziellen Bereich verfolgen. Zu den wichtigsten Messgrößen gehören die Akzeptanz des Systems durch das Personal, die Patientenzufriedenheit, die Verbesserung der klinischen Ergebnisse, die Steigerung der betrieblichen Effizienz, die erzielte Kostenreduzierung, die Verringerung von Sicherheitsvorfällen und die Datenzugriffskennzahlen. Die Forschung legt den Schwerpunkt auf die Messung sowohl quantitativer Ergebnisse als auch qualitativer Erfahrungen, um die volle Wirkung zu erfassen. Für eine erfolgreiche Messung ist es erforderlich, vor der Implementierung eine Ausgangsbasis zu schaffen und die Veränderungen im Laufe der Zeit konsequent zu verfolgen.
- Ist die digitale Transformation nur etwas für große Gesundheitssysteme?
Nein, die digitale Transformation ist für Gesundheitsorganisationen jeder Größe relevant und machbar. Während große Gesundheitssysteme möglicherweise umfassendere digitale Ökosysteme implementieren, profitieren kleinere Praxen und spezialisierte Kliniken erheblich von gezielten digitalen Tools wie telemedizinischen Plattformen, cloudbasierten EHR-Systemen und Anwendungen zur Patientenbindung. Der Schlüssel liegt in der Priorisierung von Initiativen auf der Grundlage spezifischer Bedürfnisse und verfügbarer Ressourcen, anstatt zu versuchen, das zu kopieren, was große Organisationen tun. Viele digitale Gesundheitslösungen bieten inzwischen skalierbare Preise und Funktionen, die auch für kleinere Organisationen geeignet sind.
Den nächsten Schritt in der digitalen Transformation machen
Die digitale Transformation stellt für Gesundheitsorganisationen sowohl eine große Herausforderung als auch eine enorme Chance dar. Die Beweise sind eindeutig: Technologien können die Ergebnisse für die Patienten verbessern, die Erfahrungen steigern und effizientere, effektivere Gesundheitssysteme schaffen.
Doch der Erfolg erfordert mehr als nur die Anschaffung einer neuen Technologie. Er erfordert strategisches Denken, sorgfältige Planung, nutzerzentriertes Design, robustes Änderungsmanagement und nachhaltiges Engagement der Unternehmensführung.
Erfolgreich werden die Organisationen sein, die die digitale Transformation nicht als IT-Projekt betrachten, sondern als eine grundlegende Neugestaltung der Art und Weise, wie sie Patienten und Gemeinden einen Mehrwert bieten.
Beginnen Sie mit einer ehrlichen Bewertung der aktuellen Fähigkeiten und definieren Sie eine klare Vision, die mit strategischen Zielen verbunden ist. Setzen Sie Prioritäten für Initiativen, die einen sinnvollen Nutzen bringen und gleichzeitig die Grundlage für künftige Innovationen bilden. Investieren Sie in die menschliche Seite der Transformation - Schulung, Unterstützung und Engagement sind genauso wichtig wie die Technologie selbst.
Am wichtigsten ist die Erkenntnis, dass die digitale Transformation eine Reise und kein Ziel ist. Die Technologien werden sich weiterentwickeln, die Erwartungen der Patienten werden weiter steigen, und es werden sich neue Möglichkeiten ergeben. Unternehmen, die eine Kultur des kontinuierlichen Lernens und der Verbesserung aufbauen, sind am besten positioniert, um sich anzupassen und erfolgreich zu sein.
Die Zukunft des Gesundheitswesens ist digital. Die Frage ist nicht, ob man die digitale Transformation vorantreiben soll, sondern wie man sie durchdacht, strategisch und nachhaltig gestaltet, um die bestmöglichen Ergebnisse für Patienten und Gemeinschaften zu erzielen.
Sind Sie bereit, die digitale Transformation in Ihrer Organisation voranzutreiben? Beurteilen Sie Ihren aktuellen Stand, beziehen Sie Ihre Stakeholder ein und machen Sie den ersten Schritt zum Aufbau eines vernetzten, intelligenten und patientenzentrierten Gesundheitssystems.



