Quick Summary: Digital transformation in public health leverages technology like AI, IoT, and data analytics to improve disease surveillance, health equity, and population outcomes. WHO identifies it as vital for achieving universal health coverage, with successful implementations showing increased efficiency and reduced costs. However, challenges around data governance, equity, and sustainable infrastructure must be addressed to avoid widening health disparities.
Public health systems worldwide face unprecedented challenges. Aging populations, chronic disease burdens, and emerging infectious threats demand new approaches. Digital transformation offers a path forward.
But here’s the thing—digital transformation isn’t just about adopting new technologies. It’s about fundamentally rethinking how public health functions operate, how data flows between systems, and how populations access preventive care.
According to the World Health Organization, digital transformation is vital to achieving universal health coverage. Digital technologies serve as an essential component and catalyst for enhancing sustainable health systems. The organization’s Global Initiative on Digital Health supports countries in developing robust foundations for digital health transformation that equitably strengthens health systems.
The stakes are high. In the United States alone, 75% of hospitals now use electronic health systems. This infrastructure creates opportunities for population-level insights that were impossible a decade ago.
Understanding Digital Public Health Transformation
Digital public health represents the application of digital technologies to core public health functions: assessment, policy development, resource allocation, assurance, and access. Unlike clinical digital health, which focuses on individual patient care, digital public health operates at the population level.
The distinction matters. Current digital health strategies across Canada and elsewhere adopt a primarily clinical focus, according to research published in Health Promotion and Chronic Disease Prevention in Canada. This oversight means the implications of digital technologies for public health functions don’t receive appropriate consideration.
Digital transformation in this context means more than digitizing existing processes. It requires rethinking entire workflows, data architectures, and service delivery models.
Core Components of Digital Public Health Systems
WHO’s Digital Implementation Investment Guide establishes a framework for integrating digital interventions into health programs. The framework emphasizes standardized national product catalogues and master data management processes.
These aren’t abstract concepts. They translate into practical capabilities:
- Real-time disease surveillance systems that detect outbreaks hours or days earlier than traditional methods
- Interoperable health information systems that share data across jurisdictions without manual reconciliation
- Predictive analytics platforms that identify at-risk populations before health crises emerge
- Digital supply chain architectures that ensure vaccines and medications reach communities efficiently
- Population health registries that enable targeted interventions for chronic disease management
The WHO provides stepwise guidance for developing scalable and sustainable digital health supply chain architecture. This approach adapts to specific country contexts while maintaining alignment with international standards like the SMART Guidelines.
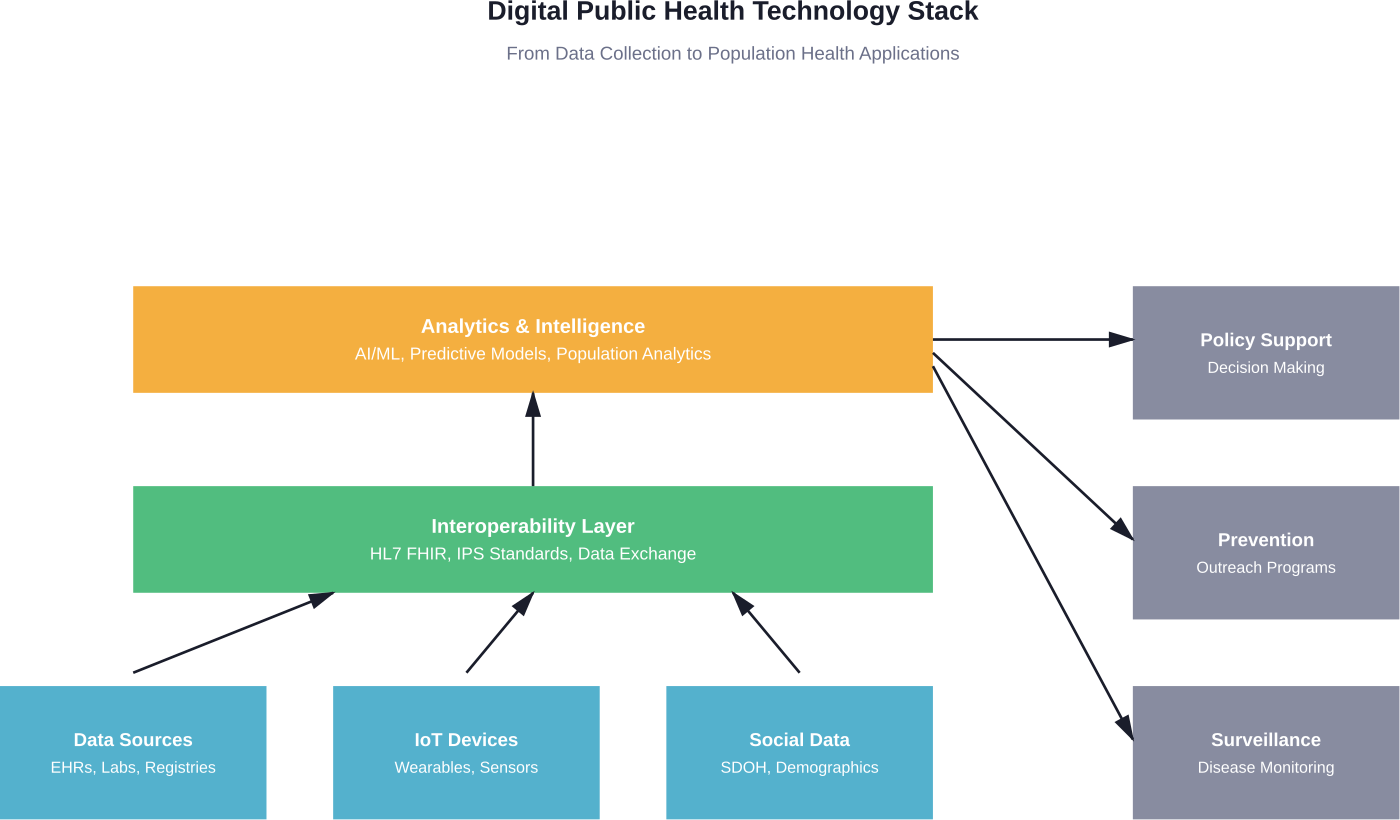
The Technology Stack
Modern digital public health relies on several interconnected technology layers. At the foundation sits data infrastructure—the systems that collect, store, and manage health information from diverse sources.
Interoperability standards like HL7 FHIR (Fast Healthcare Interoperability Resources) enable different systems to communicate. The International Patient Summary standard creates a common foundation for patient data exchange across borders and systems.
On top of this infrastructure, analytical tools process population-level data. Machine learning algorithms identify patterns. Geographic information systems map disease distributions. Natural language processing extracts insights from unstructured clinical notes.
Add Software Development Support for Public Health Projects
Public health organizations often need better internal systems, stronger data handling, and more reliable infrastructure. A-listware provides software development, IT consulting, data analytics, cybersecurity, infrastructure services, and dedicated development teams. The company can support public health projects with custom software, legacy system modernization, and extra engineering capacity.
Need a Team to Build or Support Public Health Software?
Talk with A-listware to:
- build custom software for internal operations
- modernize older systems that are hard to maintain
- add developers, data engineers, or security specialists
Start by requesting a consultation with A-listware.
Artificial Intelligence and Public Health Applications
AI’s role in public health transformation extends far beyond clinical decision support. The CDC published commentary on health equity and ethical considerations in using artificial intelligence in public health and medicine, highlighting both opportunities and risks.
The technology shows particular promise in several areas. Disease surveillance systems enhanced with AI can detect unusual patterns in emergency department visits, prescription drug sales, or social media mentions that signal emerging outbreaks.
Research published in BMC Public Health analyzed the impact of regional digital transformation on public health across 31 provinces in China. The study introduced technological innovation as a mediating variable and found significant positive effects on population health outcomes.
Practical AI Applications
Digital health transformation through AI and Internet of Things technologies is reshaping healthcare delivery globally. A 2025 study in Digital Health examined sustainable healthcare through various AIoT technology applications.
Real-world implementations demonstrate concrete benefits:
- Automated screening of chest X-rays for tuberculosis in resource-limited settings, expanding diagnostic capacity without proportional increases in radiologist staffing
- Predictive models identifying individuals at high risk for diabetes complications, enabling targeted prevention programs
- Natural language processing systems extracting social determinants of health from clinical notes, revealing upstream factors affecting population health
- Computer vision algorithms analyzing satellite imagery to identify areas with poor sanitation infrastructure or vector breeding sites
But wait. AI implementation in public health faces distinct challenges compared to clinical applications. Population-level interventions require societal agreement. Policies informed by AI—whether related to resource allocation, targeted screenings, or public health restrictions—affect people who may not directly benefit.
The CDC emphasizes that all stakeholders, from policy makers to the public, need balanced perspectives on the advantages, risks, and expenses of digital shifts. Transparent benchmarks and criteria become essential to ensure maximum benefits without marginalizing minorities or vulnerable groups.
Equity Considerations
Digital evolution poses serious equity challenges. Vulnerable populations face barriers from economic constraints, geographical isolation, or digital illiteracy. Without intentional design, digital transformation risks amplifying existing health disparities rather than eliminating them.
Research analyzing organizational digital public health strategies in Canadian provincial programs found that privacy and organizational sensitivities create barriers to data sharing and collaborative innovation. These structural issues disproportionately affect underserved communities that might benefit most from population health interventions.
Real talk: equity requires more than ensuring equal access to technology. It demands understanding how digital systems might perpetuate bias through training data, algorithm design, or implementation choices.
Data Architecture and Interoperability
Effective digital public health depends on robust data infrastructure. WHO’s handbook on digital transformation for health supply chain architecture provides stepwise guidance for developing scalable systems.
The approach emphasizes several key principles. First, standardization. Without common data formats and definitions, systems can’t communicate effectively. Second, modularity. Components should be replaceable and upgradeable without rebuilding entire systems. Third, sustainability. Solutions must function with available resources and expertise.
The Interoperability Challenge
Health data exists in silos. Hospital systems don’t talk to public health registries. Laboratory information systems use different coding schemes than immunization databases. Social service agencies track determinants of health separately from medical providers.
Standards like HL7 FHIR address these challenges by defining how health information exchanges electronically. The International Patient Summary provides a minimal set of data elements for cross-border and cross-system patient information exchange.
According to HL7, EHRs and health IT vendors are accelerating IPS adoption. The standard creates a common foundation for patient summary exchange across borders and health systems. As of August 2024, multiple EHR vendors had implemented IPS support, enabling truly interoperable health records.
The practical implications are significant. A refugee arriving in a new country could have their immunization history, chronic conditions, and medication allergies immediately available to healthcare providers. A disease outbreak investigation could rapidly pull together exposure data from multiple jurisdictions.
Building Blocks Approach
WHO’s Digital Implementation Investment Guide advocates for a building blocks methodology. Rather than monolithic systems, digital health infrastructure comprises modular components that work together.
These building blocks include:
| Building Block | Function | Examples |
|---|---|---|
| Client Registry | Unique identification of individuals across systems | Master patient index, national ID integration |
| Facility Registry | Standardized list of health service delivery locations | Hospital directories, clinic geolocation databases |
| Terminology Service | Common medical vocabularies and code mappings | SNOMED CT, ICD-10, LOINC implementations |
| Shared Health Record | Longitudinal patient data accessible across providers | Regional health information exchanges |
| Health Worker Registry | Credentials and deployment of health workforce | Provider directories, licensure databases |
This modular approach allows countries to implement components incrementally based on priorities and resources. A nation might start with a facility registry to improve supply chain logistics, then add a client registry to enable longitudinal patient tracking.
Digital Transformation for Noncommunicable Diseases
The SARS-CoV-2 pandemic demonstrated the effectiveness of rapid digital public health deployment. Digital proximity tracing apps leveraged Bluetooth capabilities to trace and notify users about potential exposures. Backed by organizations including WHO and the European Union, these tools showcased digital public health’s promise.
Now the focus shifts. Noncommunicable diseases account for the vast majority of healthcare expenses and premature disability-adjusted life years lost. Research published in JMIR Public Health and Surveillance examined digital transformation of public health for noncommunicable diseases.
The narrative for NCDs differs from infectious diseases. Chronic conditions develop over years. Risk factors span individual behaviors, social determinants, environmental exposures, and genetic predispositions. Interventions require sustained engagement rather than acute responses.
Digital Interventions for Chronic Disease Prevention
Digital technologies enable population-level approaches that were previously impractical. Mobile health applications support behavior change through personalized feedback and social support. Wearable devices track physical activity, sleep patterns, and physiological markers continuously.
But individual-level tools represent only part of the opportunity. Population health management platforms analyze aggregated data to identify communities with elevated cardiovascular disease risk. Geographic information systems map food deserts and recreational facility access. Predictive models forecast which patients will likely develop complications without intervention.
These capabilities support the core public health functions differently than traditional approaches. For assessment, digital systems provide near-real-time population health metrics rather than periodic surveys. For policy development, simulation models can estimate intervention impacts before implementation. For assurance, automated monitoring tracks whether prevention services reach intended populations.
The Human Element
Here’s the thing though—AI and digital tools can’t replace human connection in health promotion. Emotional support, cultural sensitivity, and trust-building remain fundamentally human activities.
AI serves best as a companion guiding people through the healthcare landscape. It automates repetitive tasks, freeing providers to prioritize personal interactions that can’t be digitalized. It presents individuals with tools to be proactive in their health management. But it doesn’t substitute for empathy or clinical judgment.
Research on digital health transformation published in the Journal of Healthcare Leadership examined organizational factors driving benefit realization. The study found that changes in system capabilities and organizational culture matter as much as technology selection.
Implementation Strategies and Governance
Technology alone doesn’t create transformation. Successful digital public health requires strategic planning, change management, and governance structures that balance innovation with accountability.
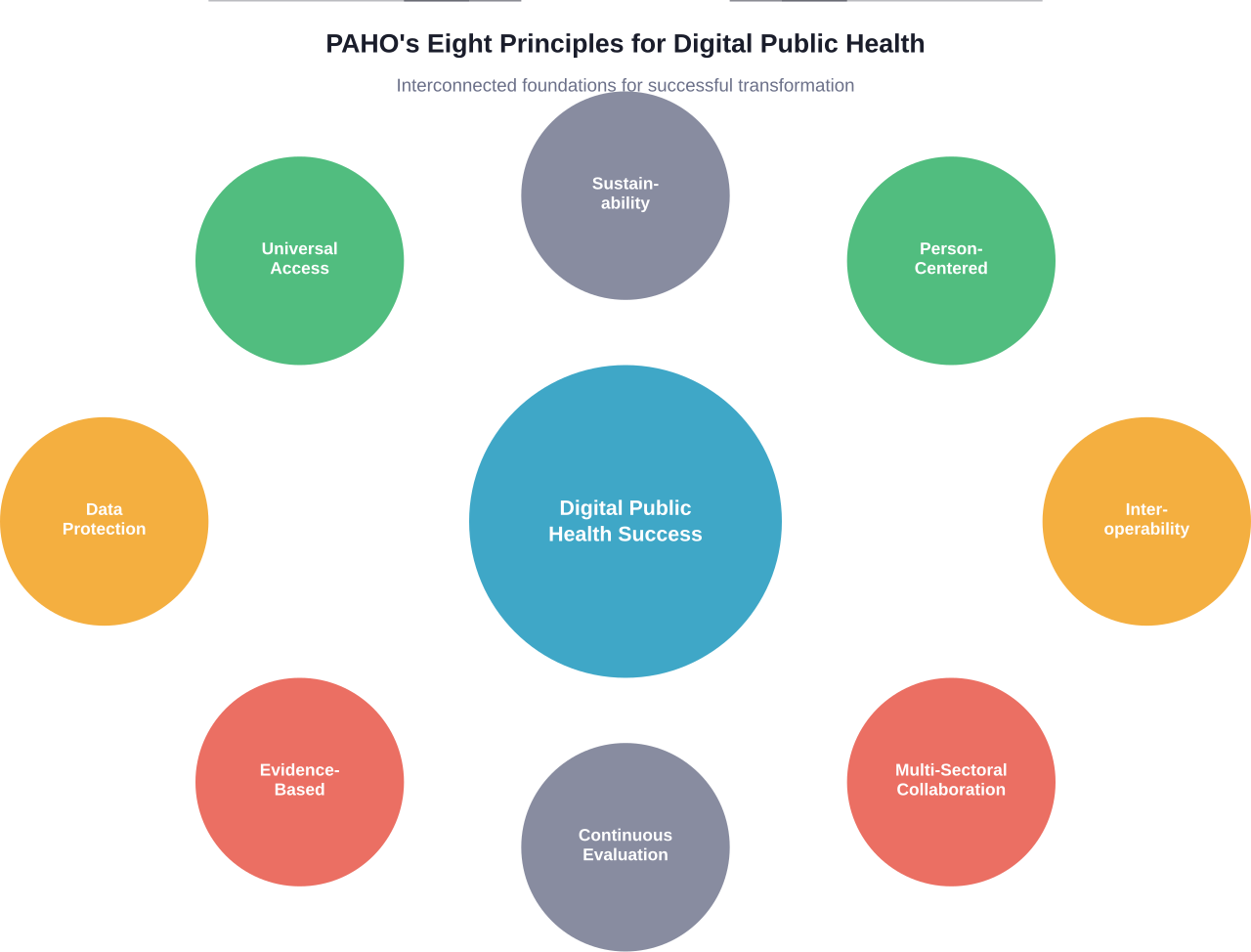
The Pan American Health Organization published eight guiding principles for digital transformation of public health. These principles address cultural changes for both health personnel and populations, aiming to support informed decision-making and sustainable public policy development.
Eight Core Principles
The PAHO framework emphasizes that digitization implies important cultural shifts.
The principles guide countries in developing short and long-term goals while ensuring no one gets left behind:
- Universal access and equity in digital health services
- Person-centered design that puts individuals and communities at the center
- Data protection and privacy as foundational requirements
- Interoperability and standardization across systems
- Evidence-based decision making using reliable data
- Sustainability through appropriate technology choices
- Multi-sectoral collaboration beyond health ministries
- Continuous evaluation and learning from implementation
These aren’t abstract ideals. They translate into concrete implementation choices. Person-centered design means involving community members in system development, not just deploying solutions designed by technologists. Data protection requires governance frameworks before collecting sensitive health information. Sustainability means choosing open-source platforms over proprietary systems in resource-constrained settings.
Organizational Readiness
Research on organizational factors driving digital health transformation benefit realization identified critical capabilities beyond technology implementation. Health service managers need new competencies in data literacy, change management, and digital strategy.
A qualitative study published in the Journal of Healthcare Leadership found that organizational improvements and changes in system capabilities are required to realize transformation benefits. Technical solutions fail without corresponding changes in workflows, culture, and governance.
Assessing digital advancement requires comprehensive frameworks. A 2024 narrative review in JMIR Public Health and Surveillance examined indicators for assessing digital public health system maturity. The study identified 286 relevant indicators from 90 references, with 46.5% having legal relevance related to big data, AI regulation, cybersecurity, national strategies, or health data governance.
Investment and Sustainability
Digital transformation requires sustained investment. In 2018, over $9 billion was invested in digital health startups by venture capital and private equity, according to research on current challenges and solutions to digital health technologies in evidence generation.
But funding digital health companies doesn’t automatically strengthen public health infrastructure. Public sector investments must focus on sustainable, scalable platforms that serve population health needs rather than individual consumer applications.
The National Academy of Medicine’s discussion paper on a national health digital and data architecture argues that the health sector lags in developing robust digital infrastructure necessary to fully realize innovations. This limits potential gains in efficiency, access, prevention, diagnosis, treatment, discovery, and public health outcomes.
Current Challenges and Barriers
Digital transformation faces significant obstacles. Understanding these barriers helps organizations develop realistic implementation strategies and avoid common pitfalls.
Technical Challenges
Legacy systems present major hurdles. Many public health agencies operate on technology platforms built decades ago. These systems can’t easily integrate with modern cloud-based applications or support real-time data exchange.
Data quality issues undermine analytics. Incomplete records, inconsistent coding, and duplicate entries create noise that obscures meaningful signals. Cleaning and standardizing data requires significant effort before advanced analytics become feasible.
Cybersecurity concerns grow as systems interconnect. Health data represents a valuable target for malicious actors. Protecting privacy while enabling appropriate data sharing requires sophisticated security architectures and governance.
Workforce and Capacity Gaps
Public health workforce capacity for digital transformation remains limited. A 2023 protocol published in JMIR Research Protocols described a multidisciplinary national health innovation research school designed to strengthen digital transformation capabilities in the healthcare system.
Doctoral students within such research schools typically acquire PhD degrees within 5 years, with approximately 80% spent on studies and 20% on organization-specific work tasks. This model recognizes that building digital public health capacity requires formal training programs, not just on-the-job learning.
Staff at all levels need new skills. Epidemiologists must understand machine learning basics to interpret AI-generated insights. Data analysts need public health domain knowledge to ask relevant questions. Program managers require digital literacy to make informed technology decisions.
Equity and Access Barriers
Digital divides threaten to worsen health disparities. Rural communities often lack broadband infrastructure necessary for telemedicine or real-time surveillance systems. Low-income populations face barriers accessing smartphones or computers required for digital health tools.
Language and literacy create additional barriers. Health information systems designed for English-speaking, college-educated users exclude significant portions of many communities. Truly inclusive digital public health requires multilingual interfaces, audio options, and simplified navigation.
Age-related digital literacy gaps affect both elderly populations and health workers near retirement. Training and support systems must accommodate diverse technology comfort levels.
Governance and Policy Challenges
Data governance frameworks lag behind technical capabilities. Questions about who owns health data, who can access it, and for what purposes remain contentious. Regulations vary across jurisdictions, complicating multi-state or international collaborations.
Privacy regulations designed for traditional healthcare don’t always address new digital scenarios. Can public health agencies use smartphone location data to track disease transmission? Should AI algorithms have access to full medical records to identify at-risk populations? These questions lack clear answers in many jurisdictions.
Procurement processes designed for physical goods struggle with software and cloud services. Lengthy approval cycles prevent agencies from adopting rapidly evolving technologies. Risk-averse purchasing rules favor established vendors over innovative startups.
Measuring Impact and Outcomes
Demonstrating value from digital transformation investments requires clear metrics and evaluation frameworks. But measuring population health outcomes presents challenges distinct from clinical effectiveness assessment.
Key Performance Indicators
Research on digital transformation in healthcare found that typical benefits include increased employee productivity, improved efficiency and effectiveness of health unit operations, and reduced operating costs.
For public health specifically, relevant metrics span multiple domains:
| Domain | Example Metrics | Measurement Approach |
|---|---|---|
| Efficiency | Time from outbreak detection to response; data entry burden reduction | Process time studies; staff time tracking |
| Effectiveness | Vaccination coverage rates; screening program reach; outbreak control speed | Program participation data; disease incidence monitoring |
| Equity | Service access disparities; digital tool usage across demographics | Stratified utilization analysis; community surveys |
| User Experience | Provider satisfaction; public engagement levels; system usability scores | User surveys; usability testing; engagement analytics |
| Economic | Cost per intervention; return on investment; resource allocation efficiency | Cost-effectiveness analysis; budget impact modeling |
The challenge lies in attribution. Population health improves due to multiple factors. Isolating the specific contribution of digital systems requires rigorous evaluation designs.
Evidence Generation Challenges
Digital health technologies have potential to improve health outcomes by increasing patient involvement in self-care, improving communication, and tailoring services to individual needs. However, generating reliable evidence about population-level impacts faces methodological challenges.
Randomized controlled trials—the gold standard for clinical research—often prove impractical for population health interventions. Random assignment of communities to digital versus traditional approaches raises ethical and logistical issues.
Alternative approaches include quasi-experimental designs comparing similar jurisdictions with different implementation timelines. Time series analyses can identify changes in trends following digital system deployment. Natural experiments leverage policy variations across regions.
Data from digital systems themselves enable new evaluation approaches. Continuous monitoring replaces periodic surveys. Granular data allows subgroup analyses impossible with traditional methods. But these opportunities require careful attention to bias and confounding.
Future Directions and Emerging Trends
Digital public health continues evolving rapidly. Several trends will shape the field’s trajectory over the coming years.
AI Integration and Large Language Models
Large language models represent a significant development for public health applications. These AI systems can process unstructured text at scale, extracting insights from clinical notes, social media posts, or scientific literature.
According to HL7’s November 2025 reflections on building standards infrastructure for healthcare AI, the rapid adoption of AI creates another pivotal moment after decades of working toward seamless health data interoperability. Standards development must keep pace with technological capabilities.
Potential applications include automated literature reviews to identify emerging health threats, chatbots providing culturally appropriate health education, and systems extracting social determinants data from diverse sources. However, ensuring accuracy, preventing bias, and maintaining human oversight remain critical challenges.
Blockchain and Distributed Systems
Blockchain technology offers possibilities for secure, decentralized health data exchange. Individuals could control access to their health information while enabling appropriate sharing for public health purposes. Supply chain applications could track pharmaceuticals from manufacture to administration, reducing counterfeit risks.
But blockchain isn’t a panacea. Energy consumption, scalability limitations, and regulatory uncertainties temper enthusiasm. Practical public health applications remain limited compared to hype.
Precision Public Health
Integrating genomic data with environmental exposures, social determinants, and behavioral factors enables increasingly targeted interventions. Rather than one-size-fits-all programs, precision public health tailors approaches to specific population segments.
This evolution mirrors precision medicine’s shift from population averages to individual characteristics. Digital systems make precision public health practical by processing the complex data required to identify meaningful subgroups and personalize interventions.
Global Collaboration Platforms
WHO’s Global Initiative on Digital Health fosters improved alignment in the digital health sector. The initiative provides governments and partners with tools, building blocks, and platforms needed for sustainable health system digitalization.
International collaboration accelerates progress. Countries can learn from peers’ successes and failures. Standards harmonization enables cross-border data exchange critical for tracking pandemics and migration-related health issues. Shared platforms reduce duplicative development costs.
The vision: countries sustainably supported to plan, resource, and develop robust foundations for digital health transformation that equitably strengthens health systems worldwide.
Practical Implementation Roadmap
Organizations embarking on digital transformation need structured approaches balancing ambition with realism. The following roadmap synthesizes guidance from WHO, PAHO, and implementation research.
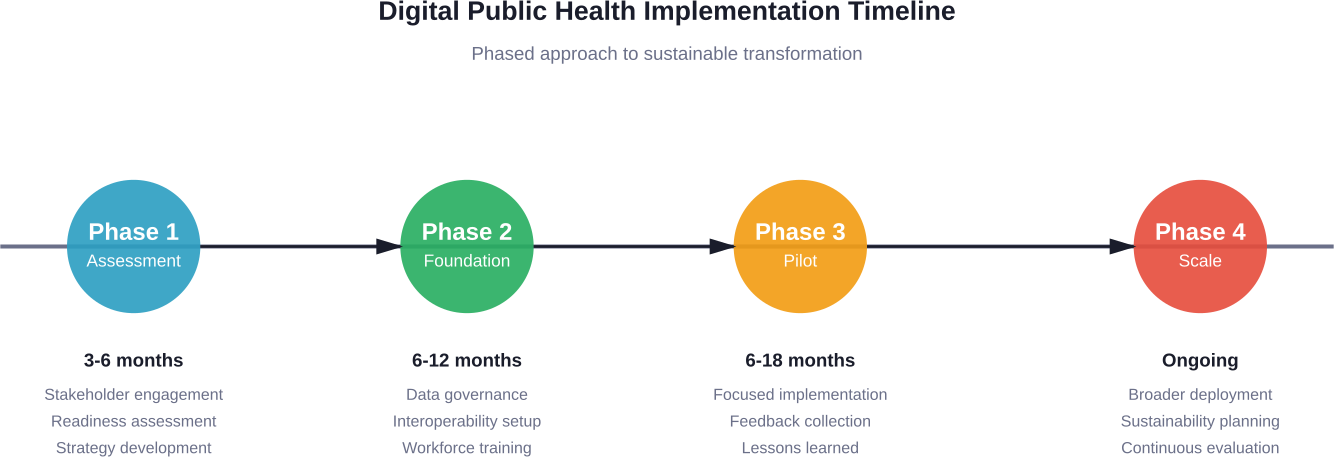
Phase 1: Assessment and Planning
Begin with honest assessment of current state. What digital capabilities exist? Where are the gaps? What organizational readiness factors need attention?
Stakeholder engagement starts here, not after decisions are made. Include frontline staff who will use systems daily. Involve community members who receive services. Consult IT professionals, privacy experts, and policy makers.
Develop a digital health strategy aligned with public health priorities. Technology serves mission, not vice versa. If childhood obesity prevention is a priority, digital investments should support nutrition surveillance, physical activity promotion, or related functions.
Phase 2: Foundation Building
Establish data governance frameworks before collecting sensitive information. Define roles, responsibilities, and decision rights. Create policies for data access, sharing, and retention. Ensure legal and ethical compliance.
Invest in interoperability infrastructure. Implement standards like HL7 FHIR for data exchange. Build or procure core registries (client, facility, provider). Establish terminology services with standard code sets.
Address workforce capacity through training programs. Develop digital literacy across all staff levels. Recruit specialists in data science, health informatics, and digital project management.
Phase 3: Pilot Implementation
Start with focused pilots rather than enterprise-wide deployments. Choose projects with clear success metrics, manageable scope, and strong leadership support. Learn from initial implementations before scaling.
Build feedback loops into pilots. Collect user experience data continuously. Monitor technical performance and identify issues early. Adjust approaches based on real-world use, not theoretical designs.
Document lessons learned systematically. What worked? What didn’t? Why? These insights inform subsequent phases and help other organizations avoid similar pitfalls.
Phase 4: Scale and Sustain
Successful pilots enable broader deployment. But scaling requires more than replicating technology. Change management, training, and support must expand proportionally.
Plan for sustainability from the start. Budgets must cover ongoing costs—maintenance, upgrades, support—not just initial implementation. Build internal expertise rather than depending entirely on external vendors.
Continuous evaluation tracks whether investments deliver expected benefits. Use data generated by digital systems to assess their own performance. Course-correct when outcomes fall short of targets.
Case Studies and Real-World Applications
Examining concrete implementations illustrates how principles translate into practice and what outcomes organizations achieve.
Regional Digital Transformation in China
Research analyzing 31 provinces in China found that regional digital transformation significantly impacts public health outcomes. The study used technological innovation as a mediating variable, demonstrating that digital capabilities enable innovations that subsequently improve population health.
The analysis revealed that provinces with more advanced digital infrastructure showed better performance on multiple public health indicators. However, the benefits weren’t automatic—they required parallel investments in workforce development and process redesign.
Canadian Provincial Public Health Programs
A qualitative study examined organizational digital public health strategy in a provincial program in British Columbia, Canada. Between February and April 2023, researchers conducted focus groups with practitioners to understand opportunities and challenges.
Participants identified several barriers to effective digital transformation. Privacy concerns limited data sharing between programs. Organizational silos prevented integrated approaches. Limited digital literacy among staff slowed adoption of new tools.
The study also revealed opportunities. Practitioners recognized that digital systems could reduce administrative burden, allowing more time for direct public health work. Improved data access would enable more targeted interventions. Automation could standardize routine processes, reducing variability.
Pandemic Response Acceleration
The COVID-19 pandemic accelerated digital public health adoption dramatically. Contact tracing apps, vaccination registries, and real-time dashboards deployed in months rather than years.
This rapid development reflected successful international collaboration and backing by organizations including WHO and the European Union. The experience demonstrated what’s possible when urgency, resources, and political will align.
However, pandemic-driven implementations often sacrificed sustainability for speed. Many systems relied on temporary funding, external consultants, or proprietary platforms. Maintaining momentum requires transitioning to sustainable models.
Frequently Asked Questions
- What is digital transformation in public health?
Digital transformation in public health means fundamentally rethinking how public health functions operate using digital technologies. It goes beyond simply digitizing paper records or adding websites. True transformation involves redesigning processes, integrating data systems, deploying analytics for population insights, and enabling new intervention approaches that weren’t previously feasible. The goal is improving population health outcomes through better surveillance, more effective prevention programs, and equitable service delivery.
- How does digital public health differ from digital health generally?
Digital health typically focuses on individual patient care—telemedicine, electronic health records, patient portals, and clinical decision support. Digital public health operates at the population level, supporting functions like disease surveillance, health promotion, environmental health monitoring, and policy development. While clinical digital health serves individual patients, digital public health serves entire communities and populations. The technologies overlap, but applications and success metrics differ significantly.
- What are the main barriers to implementing digital transformation in public health agencies?
Major barriers include legacy technology systems that can’t easily integrate with modern platforms, limited workforce capacity in data science and health informatics, inadequate funding for both initial implementation and ongoing maintenance, data governance challenges around privacy and sharing, organizational silos that prevent coordinated approaches, and equity concerns about digital divides. Additionally, procurement processes designed for physical goods struggle with software acquisitions, and risk-averse cultures resist innovation.
- How can digital transformation address health equity rather than worsen disparities?
Equity-focused digital transformation requires intentional design choices. This includes ensuring digital tools work for populations with limited internet access or older devices, providing multilingual and low-literacy interfaces, involving community members in system design, tracking utilization metrics stratified by demographic groups to identify disparities, investing in digital literacy programs for underserved populations, and maintaining non-digital service options. The CDC emphasizes that AI and digital tools in public health must avoid bias and ensure benefits reach vulnerable groups, not just privileged populations.
- What standards enable interoperability in digital public health systems?
Key interoperability standards include HL7 FHIR for health data exchange, the International Patient Summary for cross-border patient information sharing, SNOMED CT and LOINC for standardized medical terminology, ICD-10 for disease classification, and WHO SMART Guidelines for digital health interventions. These standards allow different systems—hospital EHRs, public health registries, laboratory information systems—to communicate effectively without custom integrations for every connection. Adherence to standards reduces costs and enables scalability.
- What role does artificial intelligence play in digital public health?
AI enhances public health capabilities in several ways: automated disease surveillance detecting outbreak signals earlier, predictive models identifying high-risk populations for targeted prevention, natural language processing extracting insights from unstructured text, computer vision analyzing imagery for environmental health monitoring, and chatbots providing health education at scale. However, the CDC emphasizes that AI applications must consider health equity and ethical implications. AI should augment human capabilities, not replace the relationship-building and cultural sensitivity that remain fundamentally human activities.
- How do organizations measure success of digital transformation initiatives?
Success metrics span multiple domains. Efficiency measures include reduced time from disease detection to response and decreased administrative burden. Effectiveness metrics track vaccination coverage, screening reach, and outbreak control speed. Equity indicators examine whether services reach underserved populations. User experience assessments gauge provider satisfaction and system usability. Economic evaluations calculate cost-effectiveness and return on investment. The challenge lies in attributing population health improvements specifically to digital systems versus other factors, requiring rigorous evaluation designs like quasi-experimental comparisons or time series analyses.
Conclusion: Building the Future of Public Health
Digital transformation represents more than a technological upgrade for public health. It’s an opportunity to fundamentally improve how we protect and promote population health.
The evidence is clear. WHO identifies digital transformation as vital for universal health coverage. Research demonstrates positive impacts on population health outcomes. Practical implementations show efficiency gains and expanded capabilities.
But technology alone solves nothing. Successful transformation requires strategic planning, sustained investment, workforce development, equity-focused design, robust governance, and continuous evaluation. Organizations that treat digital transformation as primarily a technology project will struggle. Those that recognize it as organizational change enabled by technology stand better chances of success.
The pandemic demonstrated what becomes possible when urgency drives innovation. Contact tracing systems, vaccination registries, and real-time dashboards deployed at unprecedented speed. This momentum shouldn’t dissipate as acute crises fade.
Noncommunicable diseases, environmental health threats, and persistent inequities demand sustained attention. Digital tools offer new approaches to these longstanding challenges—if implemented thoughtfully.
The path forward requires collaboration. International standards organizations like HL7 and WHO provide frameworks and guidance. Academic institutions build evidence and train the next generation of digital public health professionals. Technology vendors develop platforms and tools. But ultimately, public health agencies themselves must lead transformation efforts.
Sound overwhelming? Start small. Assess current capabilities honestly. Engage stakeholders broadly. Pilot focused applications. Learn from both successes and failures. Scale what works. Sustain through ongoing investment and evaluation.
The goal isn’t perfection. It’s progress toward health systems that leverage digital capabilities to serve all populations equitably. Systems that detect threats faster, prevent diseases more effectively, and allocate resources more efficiently. Systems that leave no one behind.
Digital transformation offers public health a chance to fulfill its foundational promise: improving the conditions in which people can be healthy. That opportunity demands action—strategic, equitable, sustained action.
The future of public health is digital. But more importantly, it’s human-centered, evidence-based, and committed to health equity. Technology serves these values, not the reverse.
Ready to start transforming your public health organization? Begin with assessment, engage your stakeholders, and take the first step toward a digitally enabled future that serves your entire community.



