Quick Summary: Digital transformation for healthcare payers involves modernizing operations through AI, cloud computing, and interoperability standards like FHIR to improve member experiences, reduce administrative costs by up to 30%, and enable real-time data exchange. With CMS regulatory requirements driving adoption and telehealth utilization having surged 3,800% during the pandemic, payers must shift from technology experimentation to value-driven implementation focused on outcomes, simplified communications, and integrated care coordination.
Healthcare payers are operating in an environment that’s fundamentally different from just a few years ago. The pandemic forced rapid digitalization—telehealth exploded, member expectations shifted overnight, and regulatory bodies started demanding interoperability at scale.
But here’s the thing: many payers invested heavily in digital tools without seeing the returns they expected. Bold investments were made, systems were upgraded, and apps were launched. Yet member confusion persists, administrative costs remain stubbornly high, and data still sits in silos.
The question isn’t whether digital transformation is necessary. It’s how to execute it in a way that delivers actual value—not just technology for technology’s sake.
What Digital Transformation Means for Healthcare Payers
Digital transformation in healthcare payer services goes beyond implementing new software. It’s about fundamentally rewiring operations to be data-driven, member-centric, and interoperable with the broader healthcare ecosystem.
According to CMS, the agency is taking bold steps to modernize the nation’s digital health ecosystem with a focus on empowering Medicare beneficiaries through greater access to innovative health technologies. Outdated infrastructure and disconnected data have made it harder for patients and providers to access critical information.
For payers specifically, transformation touches everything: claims processing, member communications, provider networks, care coordination, and regulatory compliance. The Centers for Medicare & Medicaid Services (CMS) has established interoperability requirements as a series of mandatory regulations (such as the CMS Interoperability and Patient Access Final Rule).
Real talk: this isn’t about chasing the latest tech trends. It’s about solving persistent operational inefficiencies and member experience problems that have plagued the industry for decades.
The Core Components of Payer Digital Transformation
Several technology pillars underpin successful healthcare payer digital transformation:
- Interoperability and data exchange: Implementing FHIR-based standards to share data seamlessly with providers, patients, and other payers
- AI and automation: Reducing manual work in claims processing, prior authorization, and member services
- Cloud infrastructure: Enabling scalability, real-time analytics, and faster innovation cycles
- Member engagement platforms: Providing transparent, personalized digital experiences through apps and portals
- Data analytics: Leveraging predictive tools to identify high-risk members and optimize care pathways
The HL7 FHIR Implementation Guide for Payer Data Exchange defines a standard interface to health insurers’ insurance plans, their associated networks, and the organizations and providers that participate in these networks. This standardization enables third parties to develop applications that help patients understand their coverage options.
Build Scalable Healthtech Solutions with Dedicated Engineering Teams
Modernizing claims processing and member engagement platforms requires specialized technical expertise and high standards for data security. Finding and retaining local talent with experience in healthcare interoperability and cloud architecture can be a slow and expensive process. A-Listware addresses this by providing dedicated development teams and IT staff augmentation, allowing healthcare payers to accelerate their digital roadmaps without the overhead of traditional recruitment.
- Niche Technical Expertise: Access to vetted developers skilled in AI, big data, and secure cloud infrastructure.
- Efficient Scaling: Quickly expand your engineering capacity to meet project deadlines or regulatory changes.
- Direct Integration: Dedicated teams that work as a seamless extension of your internal IT department.
- Resource Optimization: Reduce operational costs by utilizing a flexible, high-performance delivery model.
Start your digital transformation with A-Listware.
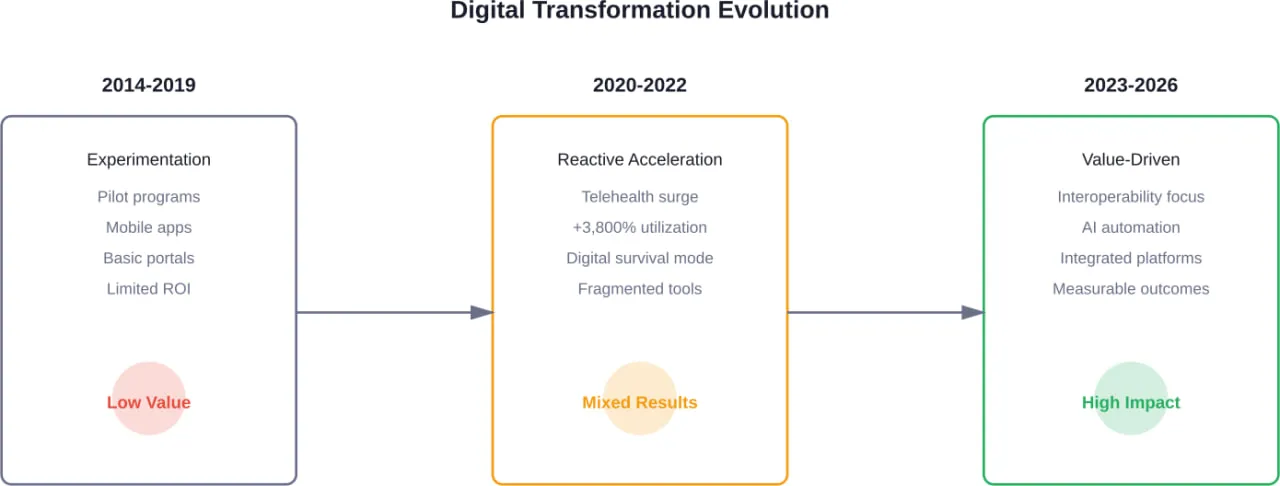
Why Payers Struggled with Early Digital Investments
The healthcare industry made bold digital investments over the past several years, accelerated by the pandemic and a growing need to modernize. Telehealth utilization rose by over 3,800% between February and April 2020 at the pandemic’s peak.
But today, many organizations are reflecting on a critical question: Are we truly realizing the value we envisioned?
Several factors contributed to underwhelming results:
- Technology without strategy. Payers deployed digital tools reactively—implementing telehealth, member apps, and home pharmacy services just to survive—without integrating them into a cohesive member journey.
- Data fragmentation persisted. New front-end systems were built on top of legacy infrastructure. Data remained trapped in silos, preventing the seamless experience members expected.
- Complex communications continued. According to research, 51% of insured adults have at least some difficulties understanding their health insurance eligibility. When members don’t understand their coverage, they make suboptimal healthcare decisions and lose trust in their payers.
The short answer? Many payers focused on digitizing existing processes rather than fundamentally rethinking how those processes should work in a digital-first world.
The Regulatory Push: CMS Requirements Driving Change
Regulatory requirements are now a major catalyst for digital transformation. The CMS Interoperability Framework represents a call to action for health data networks that want to move faster—to make what should already work, actually work.
Participation in TEFCA is voluntary for non-federal entities, but CMS mandates specific interoperability standards (API access) for regulated payers regardless of network alignment. It’s open, standards-based, and market-friendly, designed so the industry can stop theoretical planning and start executing.
Key Interoperability Mandates
CMS has established several programs and policies aimed at improving patient care through secure data exchange:
- The Promoting Interoperability Program is a quality program with the goal of driving quality improvement, safety, and efficiency of healthcare by promoting and prioritizing interoperability and the exchange of health care data through certified electronic health record technology.
- TEFCA (Trusted Exchange Framework and Common Agreement) operates in the United States as a nationwide framework for health information sharing. Created by the Department of Health & Human Services, TEFCA was designed to remove barriers for sharing health records electronically among healthcare providers, patients, public health agencies, and payers.
CMS-0057 (CMS Interoperability and Prior Authorization Final Rule) includes requirements for payers to implement FHIR-based APIs for patient data access, provider directory information, and payer-to-payer data exchange. As of January 2026, the healthcare industry continues to move from planning to active implementation of standardized data exchange, with the first phase of CMS-0057-F having taken effect.
According to Health IT data, nearly half (46%) of HIOs mapped from non-standard laboratory test or result codes to LOINC codes when accessing data from labs. Health information organizations were more likely to send data that adheres to USCDI v1 or v2, but less likely to receive data from participants that adheres to these standards.
This gap between sending and receiving capabilities highlights the ongoing challenge of achieving true bidirectional interoperability across the healthcare ecosystem.
Simplifying Healthcare Communications to Build Trust
Complex healthcare communications cause member confusion and payer inefficiencies. Simplifying products, standardizing documents, and using AI automation can improve operations and satisfaction.
The problem is significant: lack of clarity in complex, confusing language leads to misinterpretations, unexpected costs, and diminished trust between members and payers. When members don’t understand their coverage, they’re less likely to seek preventive care, more likely to face surprise bills, and increasingly frustrated with their payer.
Six Measures to Simplify Health Insurance Documents
Simplification isn’t just about plain language—it requires systematic changes to how payers structure and deliver information:
| Simplification Strategy | Implementation Approach | Member Impact |
|---|---|---|
| Standardize document templates | Create consistent layouts across all member materials | Easier navigation and comparison |
| Use plain language | Replace industry jargon with clear explanations | Better comprehension of coverage |
| Visualize complex information | Use charts, icons, and graphics for key concepts | Faster understanding of benefits |
| Personalize communications | Tailor information based on member needs and usage | Relevant, actionable guidance |
| Implement AI-powered tools | Chatbots and virtual assistants for instant answers | 24/7 support without wait times |
| Test with actual members | User testing and feedback loops before wide release | Communications that actually work |
Health insurance digital transformation can enable personalized care and proactive member guidance through integrated data. When payers connect claims history, clinical data, and member preferences, they can deliver communications that anticipate needs rather than simply responding to inquiries.
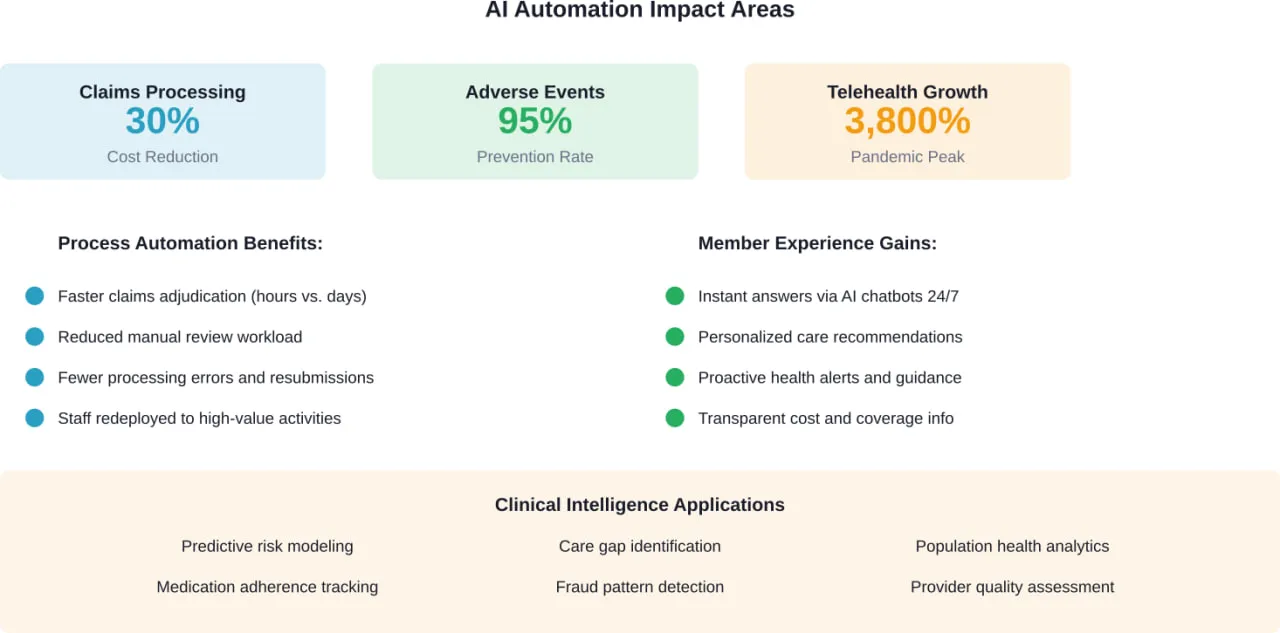
AI and Automation: Where the Real Savings Happen
Automation is where digital transformation moves from “nice to have” to “essential for survival.” When automation is scaled properly, payers can achieve up to 30% admin cost savings in claims processing.
But wait—automation isn’t just about cost reduction. It’s about redeploying human talent from repetitive tasks to complex problem-solving and member advocacy.
High-Impact Automation Use Cases
- Claims processing and adjudication. AI can review claims against policy rules, flag anomalies, and auto-approve straightforward cases. The result: faster processing times, fewer errors, and reduced administrative burden.
- Prior authorization. This has long been a pain point for providers and patients. Automated systems can evaluate requests against clinical criteria in real-time, approve routine cases instantly, and route complex cases to clinical reviewers with relevant context already assembled.
- Member service inquiries. Natural language processing enables chatbots to handle common questions about benefits, claims status, and provider networks. When escalation is needed, the system routes members to the right specialist with full conversation history.
- Fraud detection. Machine learning models can identify suspicious patterns across millions of claims—patterns that would be impossible for human reviewers to spot at scale.
By leveraging digital tools, healthcare providers can enhance the quality of care they provide and improve patient outcomes. This includes preventing up to 95% of adverse drug events and reducing duplicate testing.
Data Integration and Analytics: The Foundation
None of the fancy front-end experiences matter if the data foundation is broken. Streamlining data operations is essential for improved business agility.
Real-time data access can both speed up and improve decision-making. Digital transformation has led 65% of U.S. hospitals to use AI-assisted predictive tools embedded in their EHR systems.
For payers, integrated data platforms enable:
- Unified member profiles combining claims, clinical, pharmacy, and social determinants data
- Real-time eligibility verification and benefits checking
- Predictive analytics to identify members at risk for high-cost events
- Performance dashboards tracking quality measures and outcomes
- Population health management at scale
CMS continues to evolve Meaningful Measures 2.0 and the Cascade of Meaningful Measures framework to reflect the quality measurement priorities of the agency. When first introduced in 2017, the Meaningful Measures objective was to reduce the number of Medicare quality measures and ease the burden on measured entities.
This shift toward streamlined, meaningful measurement requires payers to have clean, integrated data that can feed reporting requirements without manual intervention.
The FHIR Standard: Making Interoperability Real
HL7 FHIR (Fast Healthcare Interoperability Resources) has emerged as the standard for health data exchange. The Da Vinci Project provides implementation guides specifically designed for payer use cases:
- Payer Data Exchange (PDex): Enables payers to share clinical and claims data with members and other payers
- Coverage Requirements Discovery (CRD): Helps providers understand coverage requirements during care planning
- Prior Authorization Support (PAS): Automates prior authorization submission and status checking
- Documentation Templates and Rules (DTR): Streamlines documentation collection for prior auth
These aren’t theoretical specifications. They’re battle-tested implementation guides with real-world adoption across major payers and health systems.
Member Experience: Personalization at Scale
Benefits of simplification include personalized products and care delivered through digital channels. Members expect the same level of digital experience from their health plan that they get from retail and banking apps.
Sound familiar? Members want to:
- Check benefits and coverage with a few taps
- Compare costs for different providers and treatment options
- Access virtual care when and where they need it
- Receive proactive guidance about preventive care and medications
- Understand their bills without needing a decoder ring
The way forward for health insurers involves building these capabilities on top of integrated data platforms. Personalization requires understanding each member’s unique health journey, preferences, and needs.
Building Effective Member Engagement Platforms
Effective member portals and apps go beyond basic features like ID card access and claims history. They provide:
- Contextual information. Rather than generic educational content, members receive information relevant to their conditions, medications, and care plan.
- Cost transparency. Before scheduling a procedure, members can see estimated costs based on their specific benefits and deductible status.
- Care navigation. Guided pathways help members find the right care at the right time—whether that’s a telehealth visit, urgent care, or specialist referral.
- Health action plans. Personalized reminders for preventive screenings, medication refills, and chronic condition management.
Now, this is where it gets interesting: when these digital touchpoints are connected to care management teams, they create a seamless hybrid experience. Digital tools handle routine interactions, while human support is available when complexity or empathy is needed.
Value-Based Care and Outcomes Measurement
Digital transformation enables payers to participate more effectively in value-based care arrangements. With integrated data and analytics, payers can:
- Track quality metrics in real-time rather than retrospectively
- Identify care gaps and coordinate outreach to close them
- Attribute outcomes to specific interventions and providers
- Share actionable insights with provider partners
- Adjust care strategies based on what’s working
The shift from fee-for-service to value-based payment models requires this level of operational sophistication. Payers can’t just pay claims differently—they need to fundamentally change how they manage populations and partner with providers.
| Traditional Payer Model | Digitally Transformed Model |
|---|---|
| Reactive claims processing | Proactive care management |
| Provider as vendor | Provider as partner |
| Volume-based payments | Outcome-based contracts |
| Annual quality reporting | Real-time performance tracking |
| Siloed data systems | Integrated health information |
| Generic member communications | Personalized engagement |
| Manual workflows | AI-powered automation |
Implementation Challenges and How to Address Them
Okay, so what about the obstacles? Healthcare payers face several significant challenges when executing digital transformation:
Legacy System Integration
Most payers operate on core administration platforms that are decades old. These systems contain critical business logic and historical data that can’t simply be replaced overnight.
The solution isn’t always rip-and-replace. Many successful transformations use an incremental approach: building modern API layers on top of legacy systems, gradually migrating functionality to cloud-based microservices, and maintaining parallel systems during transition periods.
Data Quality and Standardization
Even with FHIR standards, data quality remains a challenge. Nearly half of HIOs must map from non-standard codes to standardized formats. Incomplete member records, inconsistent provider directories, and fragmented care histories all undermine digital initiatives.
Addressing this requires dedicated data governance: establishing master data management processes, implementing validation rules at point of entry, and continuous monitoring of data quality metrics.
Change Management and Culture
Technology is often the easy part. The harder challenge is getting people to change how they work. Staff members who’ve processed claims manually for years may resist automation. Clinical teams might be skeptical of AI recommendations.
Successful transformations invest heavily in change management: communicating the vision clearly, involving frontline staff in design decisions, providing thorough training, and celebrating early wins to build momentum.
Security and Privacy Concerns
Healthcare data is among the most sensitive information that exists. Any digital transformation must maintain rigorous security and privacy protections while enabling data flow.
This requires a zero-trust security architecture, comprehensive encryption, regular audits, and privacy-preserving technologies that allow data use for analytics while protecting individual identities.
Looking Ahead: The Future of Payer Digital Transformation
As we move deeper into 2026, several trends are shaping the next phase of healthcare payer digital transformation:
- Generative AI for documentation and communications. Large language models can draft member correspondence, summarize clinical documentation for care managers, and even assist with appeals and grievance responses—all while maintaining compliance and appropriate oversight.
- Real-time benefit authorization. As interoperability matures, the vision of real-time benefit checking and prior authorization at the point of care becomes achievable. Providers get instant answers, members avoid surprise denials, and payers reduce administrative rework.
- Social determinants integration. Digital platforms are beginning to incorporate data on housing, food security, transportation, and other social factors that heavily influence health outcomes. This enables more holistic member support.
- Ecosystem partnerships. Payers are moving beyond bilateral integrations to participate in multi-party data networks. TEFCA and CMS-Aligned Networks represent the infrastructure for this connected ecosystem.
The healthcare industry continues to move from planning to active implementation. Organizations that execute well on digital transformation fundamentals—interoperability, automation, data integration, and member experience—will be positioned to lead.
Frequently Asked Questions
- What is digital transformation for healthcare payers?
Digital transformation for healthcare payers involves modernizing core operations through cloud computing, AI automation, interoperability standards like FHIR, and integrated data platforms. The goal is to improve member experiences, reduce administrative costs (up to 30% in claims processing), enable value-based care models, and meet regulatory requirements for data exchange. It’s not just about implementing new technology—it’s about fundamentally rewiring how payers operate to be data-driven and member-centric.
- Why are healthcare payers investing in digital transformation now?
Several factors are driving urgency: CMS regulatory requirements for interoperability and data exchange that took effect in recent years, the pandemic’s acceleration of telehealth and digital expectations (telehealth use rose 3,800% at peak), persistent member confusion with 51% of insured adults struggling to understand their coverage, competitive pressure from digitally-native entrants, and the opportunity to reduce administrative costs through automation. Payers that don’t modernize risk regulatory non-compliance and member attrition.
- What are the biggest challenges in healthcare payer digital transformation?
The primary challenges include integrating with decades-old legacy core administration systems, ensuring data quality and standardization (nearly half of health information organizations must map from non-standard codes), managing organizational change and culture resistance, maintaining security and privacy while enabling data flow, and demonstrating clear ROI to justify continued investment. Technical implementation is often easier than getting people and processes to change.
- How does FHIR enable payer digital transformation?
HL7 FHIR provides standardized APIs for healthcare data exchange, enabling payers to share information with providers, members, and other payers without custom integrations. The Da Vinci Project offers payer-specific implementation guides for use cases like member data access, prior authorization, coverage requirements discovery, and payer-to-payer exchange. FHIR compliance is now required by CMS regulations, making it essential infrastructure rather than optional. It allows systems to “speak the same language” for health data.
- What ROI can payers expect from digital transformation?
When scaled properly, automation can deliver up to 30% cost savings in claims processing, while AI can prevent up to 95% of adverse drug events. Beyond direct cost reduction, benefits include improved member retention through better experiences, reduced manual rework through automation, faster claims processing (hours vs. days), fewer prior authorization delays, and better performance in value-based contracts through real-time quality tracking. The key is focusing on high-impact use cases rather than trying to transform everything at once.
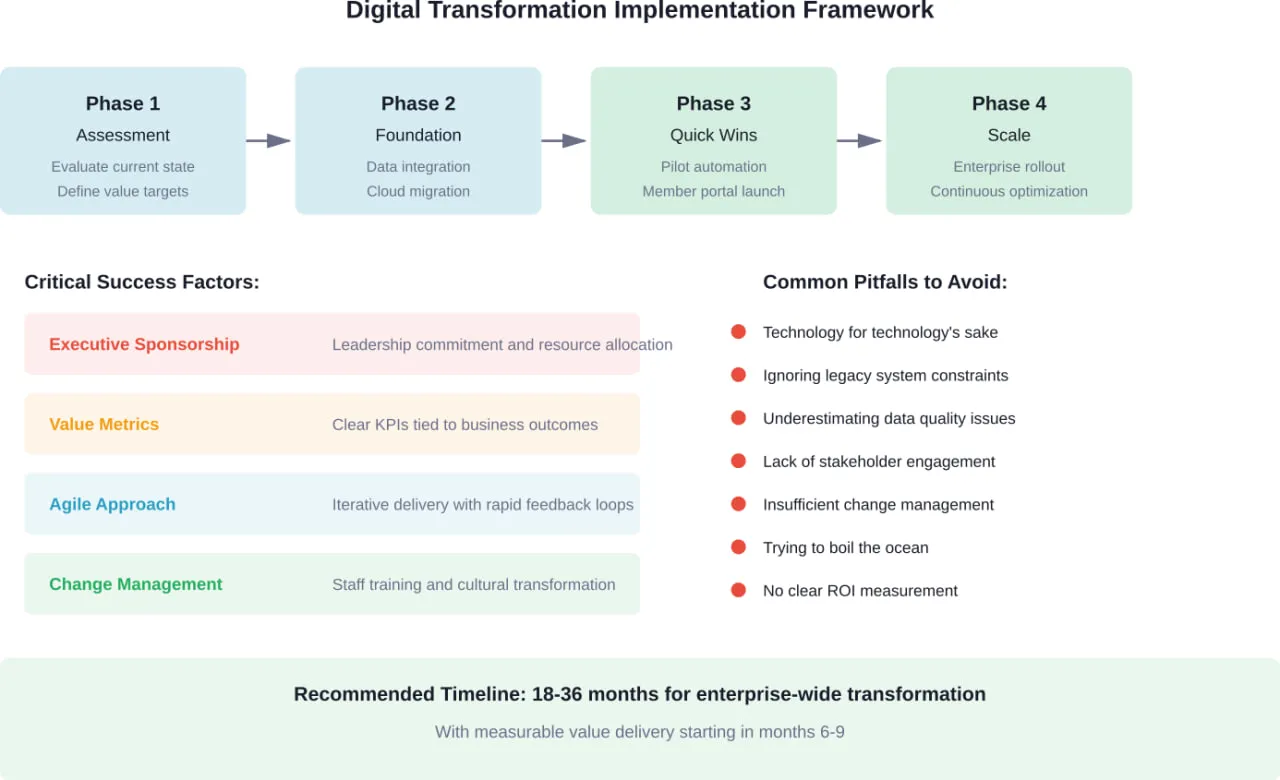
- How long does healthcare payer digital transformation take?
Enterprise-wide transformation typically requires 18-36 months, but value delivery should start much earlier—within 6-9 months for initial pilots and quick wins. The most successful approaches are phased: assessment and planning (months 1-3), foundational data and cloud work (months 3-12), pilot automation and member portal launches (months 6-15), and enterprise scaling (months 12+). Attempting to transform everything simultaneously usually fails. Incremental delivery with measurable milestones maintains momentum and executive support.
- What role does AI play in payer digital transformation?
AI powers multiple high-value use cases including claims auto-adjudication, prior authorization evaluation against clinical criteria, fraud detection through pattern analysis, member service chatbots using natural language processing, predictive modeling to identify at-risk members, personalized care recommendations, and documentation summarization. The technology has matured significantly, with 65% of U.S. hospitals now using AI-assisted predictive tools. For payers, AI enables both cost reduction through automation and quality improvement through better decision support.
Conclusion: From Strategy to Execution
Digital transformation for healthcare payers has moved from strategic aspiration to operational necessity. CMS regulations require it, members expect it, and economic pressures demand it.
The payers that will succeed aren’t necessarily those with the biggest technology budgets. They’re the ones that maintain ruthless focus on value delivery—measuring outcomes, iterating based on results, and avoiding the temptation to chase every new technology trend.
The fundamentals remain critical: interoperability that enables seamless data flow, automation that reduces administrative burden, integrated data platforms that provide a single source of truth, and member experiences that are simple, transparent, and personalized.
As the healthcare ecosystem continues evolving toward value-based care and integrated delivery models, digitally mature payers will be positioned as strategic partners rather than transactional processors. The work of transformation is challenging, but the cost of standing still is far greater.
The question isn’t whether to transform—it’s how quickly and effectively your organization can execute on the fundamentals while maintaining focus on measurable business value.


